Lung cancer stories

Explore real stories honoring survivors and those remembered through their lasting legacy. Select a category to find stories that resonate most with you.
Learn about local and national events where you can connect, raise awareness, and support the lung cancer community.
Explore real stories honoring survivors and those remembered through their lasting legacy. Select a category to find stories that resonate most with you.
Find practical advice, emotional support, and resources to help you or your loved one cope with the challenges of living with lung cancer.
Stay informed about the policies that impact the lung cancer community and ways you can get involved.
Explore breakthroughs and ongoing studies in lung cancer research, from clinical trials to cutting-edge therapies and prevention.
Catch up on highlights from our newsletter, featuring stories, resources, and upcoming opportunities to engage.
Explore news and updates shaping the lung cancer landscape—from scientific breakthroughs and organizational milestones to awareness campaigns and community highlights.


May 6, 2026

Michelle Bos-Lun is a third term state representative in the Vermont General Assembly. She lives in Westminster with her husband. She has 3 adult children and 2 grandchildren. Michelle is an enthusiastic vegan cook and baker, a mushroom forager, a hiker, and an advocate for lung cancer.
When Michelle returned home from a trip to Nepal last year, she soon found herself unable to get out of bed. At first, she thought she had jet lag, but when her symptoms worsened, she ended up in the hospital.
What followed was a whirlwind of tests and uncertainty that led to a diagnosis she hadn’t expected: scrub typhus, a rare and potentially life-threatening infection she had contracted while traveling.
But the story didn’t end there. In the process of trying to understand why she was so sick, doctors ordered a chest X-ray and saw something there that they couldn’t explain.
Three weeks and even more tests later, Michelle received a second surprising diagnosis: lung cancer.
A diagnosis she never expected
Like so many others, lung cancer wasn’t something Michelle imagined would happen to her until it did.
“Before my diagnosis, I knew of one person who had lung cancer without a smoking history,” she said. “So, while I knew it was possible, it didn’t seem at all likely. But lots of people aren’t good candidates for lung cancer, and yet it still finds us.”
Still, even in the face of a stage 3B (IIIB) diagnosis, her reaction was not what many might expect.
“I’m pretty pragmatic about things,” she said. “When something comes up, I want to learn all about it and figure out what I can do to have the best results with a situation that isn’t ideal.”
That instinct to learn, adapt, and move forward has shaped everything that’s followed

“I won the lottery”
After her initial diagnosis, Michelle entered a waiting period, one filled with a lot of questions, but few clear answers. Her oncologist couldn’t yet tell her what kind of lung cancer she had or how it would be treated. The outlook he shared at that point was sobering.
But there was one 1 possibility that offered hope, and that was a genetic mutation.
Her doctor told her, “If you have a mutation, there are some really good targeted therapies.”
Two weeks later, the call came. Michelle had ALK-positive lung cancer.
“He told me I won the lottery,” she said. “I had the best one with the best treatment.”
Within days of starting the targeted therapy, Lorbrena (loralatinib), her persistent cough, which was her only noticeable symptom, had disappeared. A few months later, her first scan showed her cancer had been reduced by nearly 50%.
“My doctor actually said, ‘This is even better than I would have expected,’” Michelle said.
A whole-person approach
From the beginning, Michelle approached her diagnosis the same way she has approached much of her life by integrating different perspectives, experiences, and tools. Having spent part of her adolescence in Taiwan, and as a long-practicing Buddhist, she was already comfortable holding multiple ways of thinking at once.
“My life has been a mixture of East and West since I was 12,” she said. “So, when I got cancer, it made sense to include a variety of different resources and approaches.”
Her treatment plan reflects that. Alongside her targeted therapy, Michelle has built a daily routine that supports her body in other ways:
- Tai Chi twice a day to improve circulation and manage neuropathy
- Walking several miles each day
- Weekly acupuncture
- Regular lymphatic massage
- A nutrient-dense, plant-based diet including daily kale smoothies, large salads, and roasted vegetables with whole grains
“I feel as healthy as I’ve ever been. Except I have cancer,” she said.
It’s a paradox she doesn’t shy away from. And it’s one she’s actively working to sustain.
“The lorlatinib gets credit for 75% of my healing, and my kale smoothies get the other 25%,” she joked.
Choosing hope—on purpose
Michelle is quick to acknowledge that everyone responds to a diagnosis differently. But for her, hope is not something she has to force; it’s something she naturally gravitates toward.
“I think you can choose to look at the hardest parts, or you can look at the possible good outcomes,” she said. “For me, it’s more satisfying to look at the positive. I try to find the best-case scenarios and aim for those.”
Even before her diagnosis was confirmed, she made a conscious choice not to dwell in pessimism.
“Before my lung biopsy, I thought, I don’t think it’s very likely that this is lung cancer, so I’m not going to worry about it,” she said. “And then when it turned out to be cancer, I said, ‘Okay, so when can we figure out how to treat this?’ I could have spent that time scared, but being scared wouldn’t have changed the outcome, only how I experienced the time leading up to it. That’s sort of how I approach everything.”
Finding community and perspective
Like many people diagnosed with a biomarker-driven form of lung cancer, Michelle quickly found community among others living with ALK-positive disease.
“I feel like I’ve been welcomed into this club that none of us wanted to join,” she said. “But since we’re here, we’re there for each other.”
Through that community, she found not only information, but perspective, including examples of people living 10, 15, even 20 years after diagnosis. Their stories helped her understand the full range of what’s possible and where she might fit within it.
“Somebody would say, ‘my husband is 21 years out’, and I thought, what? We can live 21 years with this? Knowing that some people can live quite a long time made me feel like, okay, then I can make it too,” she said.

Not waiting anymore
If there is 1 theme that runs through Michelle’s story, it’s this: don’t wait.
After her diagnosis, she began thinking about the people she hadn’t seen in years and the friendships that had drifted with time and distance. She immediately set out to rectify that. Her first trip was to reconnect with a close friend she hadn’t seen in decades.
“I just thought, I don’t want to wait,” she said. “Why did I already wait 30 years? I’m not doing that again.”
Now, her “bucket list” isn’t about places; it’s about people – reunions, visits, and time spent together.
“I hope I’m going to be around for a long time,” she said. “But in case I’m not, I don’t want to wait to spend time with the people who matter most to me. I want to see them now.”
Turning experience into action
As a state legislator in Vermont, Michelle already had a platform. After her diagnosis, she chose to use it in a new way. From the very beginning, she has spoken publicly about her experiences, using them as an opportunity to raise awareness about lung cancer, and especially the importance of early detection.
“I thought, maybe I can help somebody else,” she said. “If I can help educate someone, then go ahead, use my story.”
After her story appeared on the front page of her local paper, she learned that at least two people went to their doctors to ask for chest X-rays. For Michelle, that was enough.
“That’s the whole point,” she said.
She is also working to connect her personal experience with broader public health efforts, including initiatives that emphasize nutrition as a core component of care.
“When people eat healthy food, it helps keep them healthy,” she said. “I’m a living example of that.”
Moving forward
Less than a year into her diagnosis, Michelle’s life looks both familiar and entirely new. She is still working, still advocating, and still showing up for her family.
But she is also living with a deeper sense of urgency and intention.
“When you get lemons, make lemonade,” she said. “Well, I’m making some lemonade.”
Only in Michelle’s case, it’s likely organic, and paired with a kale smoothie.
A lung cancer diagnosis can bring a lot of questions, emotions, and uncertainty. GO2 for Lung Cancer’s free HelpLine connects you with trained specialists who can provide support, answer questions, and help you find resources along the way. Whether you’re newly diagnosed, in treatment, or navigating survivorship, you don’t have to face it alone.
Call us at 1-800-298-2436 or email support@go2.org to learn more.


May 6, 2026

For Janaki and Harsha, their wedding wasn’t just about celebrating a new chapter together; it was also an opportunity to honor the past, give back, and make a meaningful impact for others facing lung cancer.
Janaki’s connection to lung cancer is deeply personal. Her late husband, Kartik, was diagnosed with stage 4 (IV) lung cancer at just 28 years old while he was still a third-year internal medicine resident. Through a targeted clinical trial for his EML4/ALK mutation, he was able to continue working for several years before passing in 2015 at the age of 34. His journey continues to inspire Janaki’s commitment to supporting others impacted by the disease.
This was a second marriage that brought together 2 families, not starting from scratch. Material gifts didn’t feel necessary, but they knew their loved ones would still want to give something. That’s when they decided to turn their wedding into a fundraiser in honor of Kartik. “Many of our friends and family were familiar with Kartik’s journey,” Janaki said. “They were more than happy to donate, and several told us they thought it was a great idea.”
Lessons learned along the way
While their fundraiser was a success, Janaki reflects on what she might do differently.
“We didn’t initially go through GO2 because we were trying to get donations matched through companies,” she explained. “But in retrospect, it would have been easier, and likely more effective, to set up a GO2 fundraising page and link it directly on our wedding website.”
Planning ahead, she noted, could have streamlined the process and avoided fees from other fundraising platforms.
But what surprised them most was the incredible generosity of their community. “We were amazed by how much money we were able to raise.”

Tips for turning your own wedding into a fundraiser
For couples considering a similar approach, Janaki offers practical advice:
- Start early. Wedding planning gets busy, so give yourself time to set things up properly.
- Keep it simple. A direct link to a fundraising page makes it easy for guests to contribute.
- Spread the word beyond the website. Share your fundraiser at pre-wedding events or gatherings. Many guests won’t check every page on a website.
- Create in-person opportunities. If you’re hosting events leading up to the wedding, like bridal showers, engagement parties, etc, consider setting up a donation box.
- Ask for help. Friends and family are often eager to support both your wedding and your cause.
Continuing the impact
Even beyond their fundraiser, Janaki continues to connect others to GO2’s resources and recently referred a family friend for support.
“I love seeing what the organization is doing for patients and in research,” she said. “It’s providing hope and that’s one of the most important things when facing lung cancer.”
Make your celebration count
Inspired by Janaki and Harsha’s story? You can turn your own milestone—whether it’s a wedding, birthday, or special event—into a powerful way to support people impacted by lung cancer.
Start your own fundraiser benefiting GO2 and help bring hope to patients and families who need it most.
Learn more about how you can create your own fundraiser for GO2 for Lung Cancer.


May 5, 2026

For Amita Jain, MD, lung cancer is not just a diagnosis. It’s a lived experience that has shaped her life across multiple roles as a physician, a patient, a daughter, a caregiver, and an advocate.
Her family’s lung cancer story spans generations. In July 2018, her mother, Usha Jain, a retired UC Berkeley professor, was diagnosed with stage 4 (IV) non-small cell lung cancer (NSCLC) despite having no smoking history. Just 6 months later, Amita herself would receive the same diagnosis.
While both women faced advanced disease, their treatment paths diverged. Usha underwent chemotherapy and immunotherapy for nearly 2 years before stopping treatment and transitioning to routine scans. That period (often described clinically as “watch and wait”) felt anything but passive to her family.
“It was hard to feel as though we were ‘doing nothing,’” Amita recalls.
Turning to navigation for answers
As both a physician and a caregiver, Amita understood medicine, but even she found the complexity of lung cancer care overwhelming.
Navigating next steps after treatment, understanding emerging options, and keeping up with rapidly evolving research can feel like a full-time job, especially for families already carrying the emotional weight of a diagnosis.
So, Amita reached out to GO2's LungMATCH navigation program.
“I called the navigators and furnished my mom’s tumor’s genetic profile,” she says. “They reached out a day later with information on some trials for which she might qualify.”
Although her mother ultimately chose not to pursue clinical trials, the impact of that interaction was profound.
“While we did not take action on the options that the navigator provided, the information was empowering,” Amita explains. “It really helped us understand the ‘lay of the land’ in her particular situation.”
Bridging the gap between information and understanding
Even for someone with medical training, the experience revealed an important truth. Access to information is not the same as understanding it.
“Navigating is complex and scary, and getting all the information is difficult if you are not an oncologist,” Amita says. “The navigator that I spoke with was both professional and prompt. That information made me feel as though we understood our options—and that was extremely reassuring.”
For patients and families, that reassurance can be transformative.
A lung cancer diagnosis often brings not only fear, but also a sense of powerlessness. Decisions feel urgent; stakes are high, and the volume of information can be paralyzing.
“The navigator can serve as a bridge to knowledge,” Amita says. “Knowledge is power. Having a diagnosis of lung cancer can be shocking, but more importantly you do feel a bit powerless and overwhelmed. The navigators serve as a resource and lifeline.”
The invisible work of navigation
What many patients don’t see is the depth of work happening behind the scenes.
Navigators are constantly reviewing evolving research, identifying clinical trials, interpreting biomarker data, and translating complex medical information into something patients can actually use to discuss with their care teams.
“Keeping up on the information is a full-time job that most of us are not trained to do,” Amita says.
That expertise becomes especially critical at moments of uncertainty, like when treatment ends, and the path forward is unclear.
In those moments, navigation doesn’t just guide decisions; it restores a sense of control.
Strengthening navigation for the future
Stories like Amita’s mother’s underscore the critical role navigators play, not just in coordinating care, but in empowering patients and families with clarity, confidence, and connection.
To support and strengthen this role, GO2 for Lung Cancer partnered with leading experts to develop a comprehensive resource for those on the front lines of patient care.
The Lung Cancer Navigator: A Guide for Nurses and Allied Health Professionals textbook is designed to equip health professionals with the knowledge and tools they need to guide patients through every step of the lung cancer experience, from diagnosis to survivorship.
By investing in navigator education, we can ensure that more patients and families experience what Amita describes so clearly: the shift from feeling overwhelmed and uncertain to being informed and empowered.

March 30, 2026
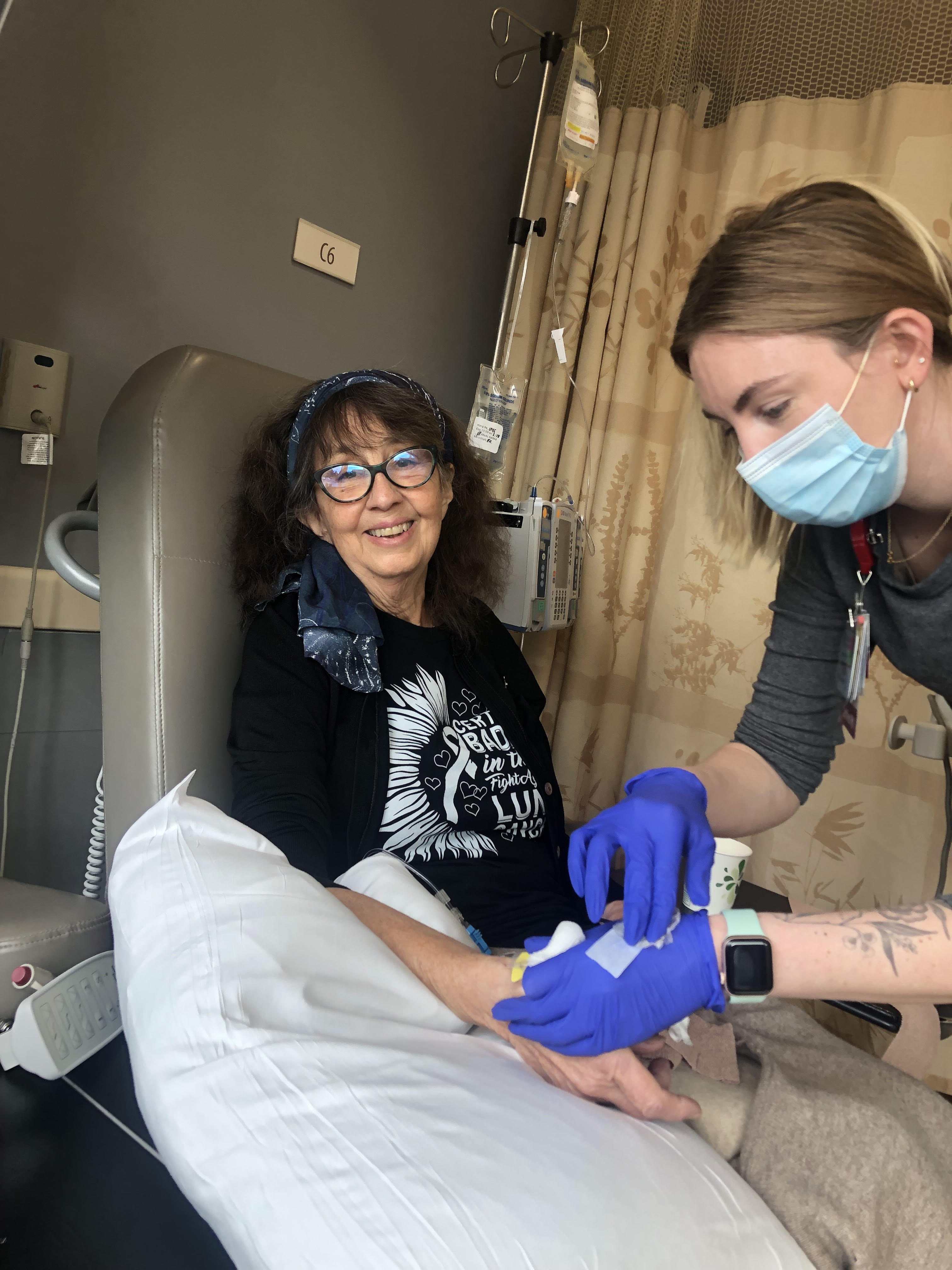
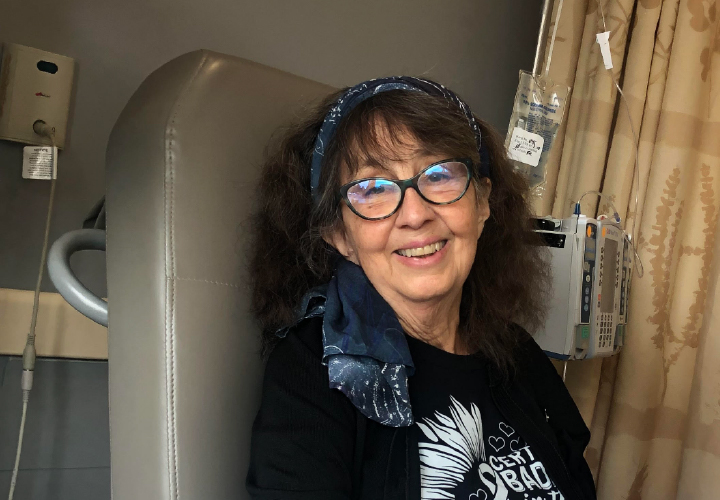
Jeanne A. lives in Hollister, CA where she is the proud guardian of her 7-year-old grandson, Joey, who she has been raising for the past 3 years. A lifelong adventurer who raised her children on Maui, HI where her grandmother was born, she still feels called to the islands, and Joey will make his first visit there this Easter. A retired social worker and current astrological teacher and counselor, Jeanne’s life is anything but quiet. She believes lung cancer may simply become 1 chapter in her story, and hopes that by sharing it, she can bring comfort to others.
An otherwise ordinary day
On a warm July afternoon in 2021, Jeanne was standing on a ladder in her backyard picking apricots when she coughed up blood. It startled her, and was unusual for her body, but she wondered if this was simply what she should expect at 72 years old since she otherwise felt just fine. Still, she called her closest friend, a nurse, and within an hour they were sitting together on Jeanne’s porch, talking it through.
Coughing up a blood clot, they ultimately agreed, was not something to ignore.
“You’d better get your affairs in order”
At the small local hospital, Jeanne was given a bed, a gown, and a long wait. Her bloodwork came back mostly normal, but hours later, when someone was finally available to read her CT scan, she was given much more shocking news: there was a 2.5-inch mass in the upper right lobe of her lung.
“You’d better get your affairs in order,” the doctor said.
Jeanne snapped back immediately, “my affairs are in order,” she said, but she was still stunned by the news. As she walked out of the ER with a brand-new diagnosis, she noticed the looks of pity on the staff’s faces — and felt something else take hold instead: resolve.
Finding the right team
Jeanne was referred to an oncologist in Salinas, CA, but she opted to go to Stanford instead. There, she met with Dr. Joseph Shrager, Professor and Chief of Thoracic Surgery, and someone she found to be calm, direct, and skilled. Early imaging suggested that the tumor might be stage 3 (III) lung cancer. Given its size, doctors worried it had already spread. There was also a small chance it could be something else entirely like Valley Fever.
The wait was agonizing, made worse by Jeanne’s history with lung cancer. Her father had died of lung cancer before his 40th birthday when she was just 5 years old. The disease had hovered in the background of her life, but now it was inside her body.
When the results came back, the answer was clear. It was not Valley Fever.
“You will Heal. It will take a while.”
Jeanne cried for a week. Then, reaching for reassurance in a place that had brought her comfort in her life, she turned to tarot cards, a practice she viewed less as prediction and more as intuition. Each time she asked what would happen, the message was the same: You will heal. It will take a while.
She didn’t fully believe it. But it helped her get through the days.
By early August, there was even more clarity as scans showed that the cancer had not spread to her lymph nodes or brain. She did, however, have a massive tumor in her lungs which Jeanne had begun calling “the Death Star.” Surgery to remove the tumor and her upper right lung lobe was scheduled for September 1.
The operation lasted hours, and Jeanne woke up with an incision beneath her right breast and drain tubes emerging from her side. She spent 5 days in the hospital, watching light move across the coastal foothills through a massive window. Healing was slow, and when Jeanne finally went home, she took with her a cough that would linger for 18 more months.
A new reality: Stage 2 (II) lung cancer
Pathology confirmed a new diagnosis: stage 2 (II) non-small cell lung cancer. Jeanne started chemotherapy nearly immediately and completed 4 rounds between October 2021 and January 2022. It was brutal for her, and during that time, she was bedridden more often than not. Her weight dropped, and her hair fell out in clumps. “It kicked my ass,” she says plainly, and she remembers very little of that time now.
Her closest friend, Annie, was there through it all. Annie drove her the 90 minutes each way to Stanford, sat beside her during infusions, brushed out the tangles when Jeanne was too weak to do it herself, and bore witness to the physical and emotional toll with quiet steadiness.
All the while, the messages from her spiritual guides remained steady. You are healing.

A different kind of hope
In January 2022, Jeanne transitioned from chemotherapy to immunotherapy as part of a clinical trial led by Dr. Joel Neal. Part of what drew her to the trial was the promise of close monitoring for 5 years and follow up for the rest of her life.
Immunotherapy was easier on her body than chemotherapy, though not without its own challenges, including unrelenting fatigue. It was worth it, though. By March 2022, there was no detectable cancer DNA in her bloodstream. Clinically, Jeanne was cancer-free, even though she wasn’t yet ready to believe it herself.
Her final immunotherapy infusion took place in February 2023. By that spring, the fog began to lift. By summer, her hair and weight had returned. And slowly, finally, Jeanne began to come back to herself.
Learning to believe it
For a long time, Jeanne practiced saying the words before she ever fully believed them. “I survived lung cancer.”
Some people say survivorship begins the moment you’re diagnosed. Jeanne understands the sentiment, but for her, accepting it took time. “Just like healing, embracing this took a while,” she says.
Then, 1 day, she looked in the mirror and finally believed it. By June, she had started telling friends, strangers, and especially the staff at Stanford Oncology, “I survived lung cancer.”
“Saying this gives real joy to people working in the field,” she noticed.
Now, Jeanne describes herself as having been “washed ashore from a wave I did not see coming and never imagined I would survive.” Her scans continue to look good. Her strength is still building. Her guides remain close. You will heal. It will take a while.
She knows now that they were right.
A lung cancer diagnosis can bring a lot of questions, emotions, and uncertainty. GO2 for Lung Cancer’s free HelpLine connects you with trained specialists who can provide support, answer questions, and help you find resources along the way. Whether you’re newly diagnosed, in treatment, or navigating survivorship, you don’t have to face it alone.
Call us at 1-800-298-2436 or email support@go2.org to learn more.


March 10, 2026

Brenda S. didn’t expect anything unusual from her visit to her primary care physician. It was the kind of routine appointment she had done many times before. It was a standard check-in, familiar questions, nothing out of the ordinary. Brenda had lived with multiple sclerosis (MS) for years and understood what it meant to manage a chronic illness, but aside from that, she considered herself healthy. Lung cancer was not on her radar.
And yet, that appointment marked the beginning of an experience that would change her life.
“You better get another opinion.”
Brenda’s experience with lung cancer stands out because it didn’t follow the path so many others know too well.
“A lot of times people are diagnosed at a pretty late stage,” she explained. “I was one of the lucky ones to get diagnosed early.”
That early diagnosis, however, didn’t come easily or immediately, and it didn’t come without persistence.
During that initial visit, something caught her doctor’s attention. Tests followed, and eventually, her doctor discovered a nodule. Brenda was told that it was benign. On the surface, that should have been the end of the story. Relief is the word most people would expect to describe that moment.
But relief wasn’t the whole truth.
“I remember just saying, please, please don’t let it be cancer,” Brenda recalled. And when she heard the word benign, she wanted to believe it completely. Yet underneath the reassurance, there was a feeling she couldn’t shake. “Deep inside, it was nagging,” she said. “It was like… I don’t know, sister, you’d better get another opinion.”
Brenda tried to move forward. Life went on. But that quiet inner voice didn’t disappear.
A gut feeling and rare early diagnosis

Brenda and her partner, Alice.
Nearly a year later, she developed a cough. It might have been easy to dismiss. After all, coughs are common, especially when life is busy and family visits. But that timing turned out to matter. Among the relatives in town was a nurse, someone trained to notice what others might overlook. She pulled Brenda’s partner Alice aside and said plainly: “This needs to be checked.”
That moment was pivotal.
Brenda listened. She followed up. And this time, the outcome was different.
The cancer was found early, something Brenda doesn’t take lightly. Early detection gave her options, time, and the ability to approach treatment without the urgency and limitations that come with a late-stage diagnosis. She knows how rare that is in lung cancer, and she doesn’t call herself lucky casually.
Her story is a reminder that diagnosis is not always a single moment, but a series of decisions—some small, some difficult—that add up. It’s about trusting medical expertise, yes, but also trusting yourself. Brenda’s experience underscores how critical self-advocacy can be, especially when something doesn’t sit right, even if the initial answer seems reassuring.
Living fully

Beyond her diagnosis, Brenda is someone defined by far more than cancer. One of the joys woven throughout her life has always been singing. Whether performing when she was younger or sharing music in more personal settings, singing has long been part of who she is. Today, Brenda has found her way back to jazz singing, a return that feels especially meaningful. Being back in that space, reconnecting with music and performance, has brought her renewed joy and vitality. Singing is an expression of creativity, resilience, and presence, qualities that carried her through uncertainty and continue to ground her now.
Cancer has a way of narrowing focus, of making life feel smaller. Brenda’s story pushes back against that. It’s not just about what she faced, but about how she continues to live fully, with gratitude and purpose. Returning to jazz is not about going back to who she was before but embracing who she is now. She speaks openly, not because the moments leading to her diagnosis were easy, but because she hopes her experience might help someone else pause, ask another question, or seek a second opinion when something feels off.
She’s also quick to express appreciation for her doctors, for her family, and for the advocates and organizations working to change the lung cancer narrative. “Thank you to GO2 for Lung Cancer for the work you are doing,” she said. “I’m here, whatever I can do.”
Brenda’s experience is a powerful reminder that early detection saves lives, that listening to your instincts matters, and that sometimes the most important voice to hear is the quiet one telling you to look again.
GO2’s HelpLine is a free, one-on-one service that connects patients and caregivers with experienced staff who can provide guidance, resources, and, most importantly, hope. Whether it’s questions about getting a second opinion, biomarker testing, screening, treatment options, or simply needing someone to listen, the HelpLine is here to make sure you know you are not alone. Call 1-800-298-2436 or email support@go2.org to get started.


March 3, 2026

When Rachel S. talks about her mom, Jan, you can still feel the energy she brought into every room. Jan was hilarious, dramatic in the best way, endlessly curious, and deeply kind, the type of person who made everyone feel special. She loved through food, through knitting, and through gathering people together.
In late September 2024, Rachel and her family were blindsided by a stage 4 (IV) lung cancer diagnosis. Just months later, on January 17, 2025, Jan passed away. The loss was sudden and devastating, but her spark never faded.
Today, Rachel and her family honor Jan’s life by coming together each year at GO2’s Sacramento 5K Walk/Run in her memory, turning grief into connection and action. We sat down with Rachel to learn more about her mom’s life, legacy, and the impact she continues to have on everyone who loved her.
Tell us about Jan
If I were introducing my mom at a gathering, there’s a strong chance people would already know her – or she would have already made herself known. She was genuinely hilarious. The kind of person who could tell a story and have an entire table crying with laughter. She was loud in the best way, dramatic, animated, obsessed with true crime, and completely unafraid to strike up a conversation with anyone. People loved her. I mean truly loved her. She had fans. But underneath all of that personality was someone deeply kind and interested in people. She made you feel special. That was her magic.
What were some of the things she was most passionate about – hobbies, traditions, routines, or little quirks that made her her?
After I left for college, her best friend taught her to knit. That turned into hundreds of beanies and blankets for family, friends, grandchildren – even cancer organizations. She was also the quintessential Jewish mom – an incredible cook and host. Holidays and gatherings at our house were sacred. Feeding people was how she loved them.

Can you share a moment or memory that feels especially representative of who she was?
My mom would move mountains for my sister and me. In 1998 she surprised us with Backstreet Boys tickets and a trip to Las Vegas – and then surprised us again with a second night and front row seats. That kind of over-the-top joy was so her. After she passed, they announced a Vegas residency, and my dad, sister, and I went. It felt like she made it happen.
When she was diagnosed, what do you remember most about that time – emotionally or practically — for your family?
It was a living nightmare. One day she was healthy, and the next we were told it was stage 4 (IV) lung cancer. By the time we had answers in late September, tumors had fractured her spine, and she was in bed until she passed on January 17, 2025.
Everything was hard. She couldn’t move, so every appointment required enormous coordination. We were incredibly fortunate to have neighbors and lifelong friends who stepped up in extraordinary ways.
Even with that support, it was overwhelming. There are so many unknowns with a diagnosis like this, which is why guidance and community around lung cancer matter so much.
How did she approach life in the months that followed her diagnosis?
She was still herself. Sassy. Funny. Curious. Even from bed, she wanted to know all of the gossip. She still made jokes. That spark never left her.

What kind of impact did she have on her family, friends, and neighbors?
The number of people who showed up for her and for us told me everything I needed to know about her impact.
She built real relationships. With neighbors. With lifelong friends. With our friends. With people she met once and somehow remembered forever. She made people feel seen and important. That kind of energy doesn’t disappear.
Since her passing, how have you seen her legacy live on in your family or community?
Her knitting is everywhere. Her recipes are still in rotation. We still host. We still gather.
But more than anything, she changed how we live. There’s a depth now. A perspective you don’t get unless you’ve experienced loss like this. We don’t sweat the small stuff the same way anymore.

Can you describe what motivated you to participate in GO2’s Sacramento 5K Walk/Run in her honor?
Grief is disorienting. I needed community and I needed direction. I needed to turn heartbreak into action. If I couldn’t save my mom, I wanted to help save someone else’s. Leading the 5K in her honor felt like the most meaningful way to do that.
What does it mean to you to have family and friends come together at this event to celebrate her life?
We formed our team just a month after she passed. It was still so raw, but we needed it.
Seeing that many people show up for her – walking, donating, wearing her name – was incredibly healing. It reminded us how much she meant and that we were helping fund real progress in her honor.
How does this event help shift the narrative around lung cancer from loss and stigma to community, celebration, and hope?
Cancer is everywhere. It’s happening younger. It’s happening to nonsmokers. It’s happening to people who “did everything right. “Events like this help dissolve isolation. They replace stigma with community. They remind families that they are not alone. And, they fund real progress.
Grief can be incredibly lonely. This makes it collective, and collective grief can become collective hope.

If you had to sum up what you hope readers understand about your mom, what would you want them to take away?
There will never be enough time with the people we love. My mom lived loudly, generously, and with joy. I hope people step away from the noise of daily life and remember that right now is what we have. Don’t wait to show up. Don’t wait to say the thing. Live bigger while you can.
Honor your loved ones by joining a GO2 5K Walk/Run near you, or by starting your own team. Every step helps fund programs, research, and resources that ensure no one faces lung cancer alone. Find an event and join us!


March 3, 2026

Glen lives in Hercules, CA with his Yorkie, Kuma, where he moved in 2021 to be closer to family and friends. After nearly 20 years working in the probation department, he retired at the beginning of the pandemic and began volunteering at the East Bay SPCA. What started as a way to give back quickly turned into a full-time job. These days, you’ll often find him on his daily walk to Starbucks or visiting his mom, who lives just 15 minutes away.
Jeffrey B. Velotta, MD, FACS is a thoracic surgeon at Kaiser Permanente’s Oakland Medical Center, a Clinical Professor in the Department of Clinical Science at Kaiser Permanente’s Bernard J. Tyson School of Medicine, and a clinical assistant professor in the Department of Surgery the UCSF School of Medicine. Dr. Velotta went to medical school at George Washington University. He then completed his general surgery residency at UCLA Medical Center. During this time, Dr. Velotta also completed his postdoctoral research in the Department of Cardiothoracic Surgery at Stanford University School of Medicine. Following this, he completed his training in Cardiothoracic Surgery at Brigham and Women’s Hospital and Harvard Medical School. Dr. Velotta’s clinical and research interests involve innovative techniques and regionalization pathways for all thoracic cancers and improving lung cancer screening in at-risk populations.
When Glen first noticed chest pain in the fall of 2024, lung cancer wasn’t on his radar. He was in physical therapy at the time and assumed the discomfort was muscular and temporary. But 1 test led to another, and by December, an X-ray raised concerns that couldn’t be ignored.
On December 24, 2024, Glen had a biopsy. Four days later, he received a phone call confirming cancer.
“I didn’t know what stage I was or much about what I was even being diagnosed with,” Glen recalls. “I just know it turned my world upside down.”
Glen didn’t have a smoking history, and there was no history of lung cancer in his family. Yet here he was, grappling with a diagnosis he never expected and didn’t yet fully understand.
Hearing the worst news, but not much else
Glen remembers little of the conversation that followed his diagnosis. His oncologist delivered the news with compassion, giving him permission to react however he needed.
“She said, I’m telling you the worst news I could possibly tell you. It’s okay if you get upset, scream, or cry. I’m here,” he says.
But like many patients in that moment, Glen fixated on 1 question: How long do I have to live? “I wasn’t really hearing anything else,” he says. “My best friend was with me, taking notes. I’m glad she was there because I don’t remember much of what was said. I could only think about my prognosis.”
In the days that followed, Glen did what so many people do, he went online. And almost immediately, he regretted it. “That was the worst thing I could do,” he says. “You Google stage 4 (IV) lung cancer and life expectancy, and the first article you see tells you that this is really bad news. You don’t even need to read the rest.”
Treatment, side effects, and a growing sense of fear
Glen began treatment quickly. His first regimen included radiation to his brain and chest and an infusion therapy that caused repeated breathing reactions. After 4 reactions across 2 sessions, his care team stopped the drug. He later transitioned to Tagrisso (osimertinib), which he is still on today and has tolerated much better.
But emotionally, Glen was spiraling. He describes himself as generally relatively pessimistic by nature, and the statistics he’d read didn’t help. He began quietly preparing for the end, updating legal documents, organizing passwords, and making sure his affairs were in order.
A parking lot, a 5K, and an unexpected meeting
Everything began to shift at GO2’s San Francisco 5K Walk/Run. Glen attended the event almost on a whim after finding information about it online. He arrived early, sat in his car, and debated leaving. Eventually, he got out and walked toward the event, unsure why everyone seemed so happy. “This is a cancer walk,” he remembers thinking. “Why is everyone smiling?”
A volunteer noticed he wasn’t okay and introduced him to GO2’s Senior Manager, Support Programs and Events, Michele Zeh. As Glen shared how bleak he was feeling, she pointed around the room. “This person has 10 years since their diagnosis. That person has 8,” she told him.
“And I’m thinking, how is that possible? I thought people never lived that long,” Glen says.
Then Michele asked a simple question: “Do you know Dr. Velotta?”
Glen didn’t. But meeting him was about to change his life.
“Let’s get rid of the mothership”

Dr. Jeffrey Velotta is a thoracic surgeon at Kaiser Permanente in Northern California, and one of only a small number of surgeons in the country willing to seriously consider surgery for patients with stage 4 (IV) lung cancer.
When Glen met him, the conversation felt different immediately. “He really cared,” Glen says. “I could tell right away how passionate he was about lung cancer and about the people who have it. It made me feel good.”
Dr. Velotta reviewed Glen’s scans and told him that he could be a good candidate for surgery, a treatment that might help his prognosis despite his stage 4 (IV) diagnosis. He explained his thinking using an analogy that stuck.
“We’ll get rid of the mothership,” he said.
The primary tumor, Dr. Velotta explained, was like a command center that was sending cancer cells elsewhere. If Glen’s metastatic disease was controlled with medication, removing the original tumor could still slow or stop future progression.
“The approach made sense to me,” Glen says. “You’re radiating my brain and my bones but you’re leaving where it all started? Why not get rid of that, too?”
Why surgery for stage 4 (IV) is still so controversial
Dr. Velotta is blunt about how unusual his approach still is. “I don’t think every patient with stage 4 (IV) lung cancer should have surgery,” he says. “But I absolutely believe that some should, including many more than most doctors currently consider.”
In addition to being younger, healthier, and generally fit, the key factor that makes someone a good candidate, he explains, isn’t the extent of the disease or the number of metastases, but whether disease outside the lung is controlled.
“Glen had multiple spots in his brain, bones, and elsewhere,” Dr. Velotta explains. “But his cancer was well-controlled through a tyrosine kinase inhibitor (TKI). That’s what people call ‘polymetastatic’ disease. Most surgery trials exclude patients like that. But that’s actually the majority of people with stage 4 (IV) lung cancer.”
Clinical trials, he notes, tend to focus on patients with 1 or 2 metastases, not because others can’t benefit, but because trials are designed to show clean, easily publishable results. This disconnect, he believes, is 1 of the reasons surgery remains underused for people with advanced disease. “That leaves most patients out,” he says. “And it leaves surgeons hesitant.”
A lonely position in the field
Even today, Dr. Velotta says the prevailing mindset around surgery for stage 4 (IV) lung cancer hasn’t shifted much. “The thinking is that it’s too little, too late. We’ve missed the chance to help these patients surgically. The idea is that the cat’s already out of the bag,” he says.
That assumption, that surgery can’t help once cancer has spread, is something he pushes back against constantly. “People get freaked out by polymetastatic disease,” he says. “They see multiple spots and think, ‘Oh my God, they’re everywhere.’ But if those spots are controlled, it doesn’t matter how many there are. Those patients can still benefit.”
Dr. Velotta acknowledges that his willingness to operate in these cases often puts him at odds with colleagues. “There is a stigma associated with operating on stage 4 (IV) lung cancer,” he says.
Even within his own health system, he is frequently the only surgeon willing to consider surgery for patients like Glen. “I feel very alone in this world sometimes,” he admits. “If these patients were all doing terribly, I would stop. But they’re actually doing really well.”
Instead, he says, many of his patients are living longer — and living well. “I’ve done this for 5 or 6 years. I’ve operated on many,” he says. “A lot of them are still alive. And even the ones who passed didn’t pass 3 months later. Some lived 6 plus years.”
Surgery as more than survival statistics
For Glen, surgery wasn’t just about controlling the disease. It was about reclaiming a sense of control over his own life. Surgery felt proactive to him, like taking control of his treatment and his future.
Dr. Velotta sees that psychological impact again and again. “You can’t quantify that on a spreadsheet,” he says. “But mentally, it matters a lot.”
Glen agrees. “I felt better from the moment I knew I was going to have surgery,” he says. “I can’t put that on paper, but I felt different. Better. It has helped my mindset immeasurably.”
Glen had surgery on November 12, 2025. It was minimally invasive, and he went home 2 days later. Within weeks, he was walking hills near his house. Then jogging. Then biking.
“I’m not back to where I was yet,” he says. “But I’m close. And I really don’t mind putting in the work.”
Pathology from his surgery showed just .5 millimeters of active cancer remaining in the tumor that was removed. “All I cared about was that it wasn’t inside me anymore,” Glen says.
NED — and what hope looks like now

When Dr. Velotta emailed Glen with the words “NED” or “no evidence of disease,” Glen didn’t fully grasp what it meant, but others did. “When I told people at GO2, they got really excited,” he says. “That’s when I realized, oh, this is a big deal.”
Hope, he says, is everything. “Sometimes I’m still pessimistic at heart,” he admits. “But the surgery has given me so much more reason to have hope for the future, and hope is what keeps me going.”
On sharing his story
Glen hesitated before agreeing to speak publicly about his experiences with lung cancer. Talking about cancer can still pull him into dark places. But ultimately, he agreed for 1 reason.
“If this helps 1 person,” he says. “If someone like me hears this and thinks, ‘Maybe surgery is an option for me, maybe I should ask’, then it’s worth it.”
Dr. Velotta agrees. “I just want people to know that they can ask,” he says. “That’s huge progress.”
GO2’s HelpLine is a free, one-on-one service that connects patients and caregivers with experienced staff who can provide guidance, referrals, resources, and, most importantly, hope. Whether it’s questions about biomarker testing, treatment options, or simply needing someone to listen, the HelpLine is often the first step toward feeling less alone after a lung cancer diagnosis. Call 1-800-298-2436 or email support@go2.org to get started.


February 3, 2026

When Mike Scanlon set out on a 30-day, 700-mile bike ride across Kansas, the journey ahead of him was daunting. He had 60 trails, 50 towns, and what felt like endless gravel roads ahead of him. But for Mike, who is living with stage 4 (IV) non-small cell lung cancer (NSCLC), this ride was about more than just the distance. It was about purpose and about transforming his diagnosis into something bigger.
At the heart of Mike’s journey was a principle that has guided his work and his life for years: the Athenian Oath, a commitment to leave things “not less, but greater, better, and more beautiful than they were transmitted to us.” Turning his ride into a fundraiser for GO2 for Lung Cancer and Kansas Trails Inc. was a natural extension of that belief. “I’ve always tried to live in a way that gives back,” Mike shared. “This ride felt like a way to do that — to take something personal and make it meaningful for others.”
Choosing “even if” over “only if”
Mike often described the Ride for Resilience tour as a lesson in mindset. It was one shaped deeply by his cancer diagnosis. Living with stage 4 (IV) NSCLC, he explained, can trap people in “only if” thinking: “I’ll have peace only if treatment works. Only if scans stay clear. Only if life goes back to normal.”
But the road taught him another way.
“The power of an ‘even if’ perspective is that it frees you to live with purpose no matter what happens,” Mike said. “Even if the road is uncertain. Even if outcomes aren’t guaranteed. Even if this journey reshapes your life.”
For Mike, resilience wasn’t about controlling the outcome. It was about choosing courage anyway. Pedal after pedal, day after day, that mindset carried him forward.
Trails, towns, and the strength of small places
Kansas is home to more than 4,000 miles of trails, and Mike wanted to experience as much of that diversity as possible. Riding 60 trails across 50 towns allowed him to connect not just with landscapes, but with people — especially in small, rural communities.
“I wanted to see how adaptable and resilient these towns are,” he said. “A lot of them don’t have much, but they keep showing up.”
That resilience came into sharp focus in places like Copeland, KS, population 251. A stop at the town library became a powerful reminder of shared values and of communities that quietly live out the Athenian Oath and the “even if” mentality every day. These towns, like people facing cancer, keep moving forward despite uncertainty.
Sharing the road and stories

Along the way, survivors, caregivers, and families found Mike. Sometimes it was literally on the trail, sometimes through word of mouth. They rode beside him and shared their stories.
Over the course of the ride, Mike connected with people across Kansas, creating space for honest conversations about cancer, treatment, and hope. He shared information about GO2 for Lung Cancer, including resources available to individuals and families at every stage of the disease.
“Cancer is deeply personal,” Mike reflected. “The courage it takes for people to open up always floored me.”
From a sales director at a Salina radio station to an administrative assistant at a high school in Wamego — who happened to share Mike’s same lung cancer mutation and treatment — these conversations became some of the most meaningful moments of the ride.
Hard miles and harder questions
The ride tested Mike in ways he didn’t expect, including fast farm dogs on gravel roads (most of which he could outpace, except one). But the hardest challenges weren’t physical. They were mental.
“I’ve been given an opportunity many people with NSCLC don’t get,” he said. “And I can’t waste it.”
A note from a donor, a message of encouragement, or simply the mantra JKP — Just Keep Pedaling — helped him find the answer.
The ride of a lifetime

The final day was a 93-mile ride along the Flint Hills Trail from Council Grove to Osawatomie felt symbolic. Mike saw the day as a reflection of life itself: starting early, uncertain, learning as you go, growing stronger, then feeling your body push back near the end.
And then, 2 miles from the finish, everything changed.
“I saw my grandson, Augie,” Mike said. “He wanted to ride the last 2 miles with me. And I knew his little brother PJ was waiting at the finish line with my daughter Megan.”
As Mike’s journey that day ended, his grandsons’ life journeys were just beginning, bringing the Athenian Oath full circle. “My obligation,” Mike said, “is to transmit Kansas trails — and this life — not less, but greater.”
Your turn to find your “Ride for Resilience”
Mike’s advice to anyone considering a fundraiser for GO2 for Lung Cancer is simple: define your reason.
“Mine was the Athenian Oath,” he said. “Once you know your why, invite others to help.”
Through his 700-mile journey, Mike raised more than $24,000, helping fuel GO2 for Lung Cancer’s work to increase lung cancer survival by supporting cutting-edge research, legislative advocacy, and patient support services for individuals and families nationwide.
Whether it’s a ride, a walk, a creative challenge, or something uniquely yours, your fundraiser can make a difference. As Mike’s journey shows, resilience isn’t about what happens only if everything goes right — it’s about choosing to act, even if the road ahead is uncertain.
And sometimes, all it takes is the courage to start pedaling.
Learn more about how you can create your own fundraiser for GO2 for Lung Cancer.


February 3, 2026

June & Roy live in Kennebunk, Maine, a place they moved after visiting and vacationing many times throughout their lives. They enjoy barefoot beach walks, snowshoeing, many volunteer activities focused on environmental issues, Indigenous People’s rights, social justice issues, and textile drives organized by June which have kept over 20 tons of textiles and footwear out of landfills. They also enjoy exploring Maine’s forests and mountain areas. June is a retired clinical registered dietician while Roy is a retired banking executive and director. They see a return trip to Switzerland and other excursions in their future. Their favorite toast with an adult beverage is “Ein Sache”, followed by “Uns” — German for “One Thing” and “Us”. Roy is still trying to find where June hid his heart when she stole it. She promises him that it’s in a safe place.
After a history of heart disease, Roy has learned to pay attention to his body, so when he experienced shortness of breath in July 2018, he went to the emergency room. This time, his heart wasn’t his problem. Imaging revealed a large mass in his upper right lung and, with it, a diagnosis that would reshape his years ahead.
Doctors moved quickly. A biopsy confirmed lung cancer, and additional scans showed it had spread to nearby lymph nodes, ruling out surgery. Roy was referred to David Carbone, MD, PhD at The James Comprehensive Cancer Center, where a treatment plan came together quickly.
Roy enrolled in a clinical trial led by Dr. Carbone to explore using immunotherapy in people with stage 3 (III) non-small cell lung cancer (NSCLC). He would receive immunotherapy, then radiation, then chemo, and then immunotherapy again.
The early months were manageable, and Roy didn’t experience any side effects during his initial immunotherapy infusions. Radiation and chemotherapy followed, spaced carefully over many weeks. But toward the end of treatment, a rare and severe reaction to chemotherapy landed Roy in the hospital for 10 days.
This experience forced difficult treatment decisions and required Roy to advocate for himself, something he had learned to do years earlier while caring for his late wife during her illness. Immunotherapy was paused, then ultimately stopped altogether, when Roy developed serious gastrointestinal side effects. By that point, his treatment had already achieved a complete response, and his body could not tolerate continuing.
With treatment complete, Roy entered a new phase: survivorship, including regular monitoring and cautious hope. Follow-up scans initially came every 6 months, then 9, then eventually once a year.
Judy’s story
Roy’s experience with lung cancer was not his first time navigating serious illness. Just a few years earlier, he had walked a parallel path alongside his late wife, Judy.
In November 2015, Judy collapsed in their shower at their home in southeastern Ohio. At the hospital, imaging revealed a large mass in her brain. Judy immediately understood what that meant. Her aunt had died of glioblastoma years earlier, and Judy had been one of her caregivers.
Judy underwent brain surgery the day before Thanksgiving, followed by months of treatment including clinical trials, aggressive chemotherapy, and a 2nd surgery. Despite everything, Roy remembers her determination to keep living fully and authentically, even as options narrowed.
Judy approached her illness with the same intention and creativity that defined her entire life. A spiritual director and artist, she continued creating throughout her treatment, painting, weaving, and writing as a way to make meaning of what she was experiencing. Even after a stroke affected her body’s complete left side (she was left-handed), she adapted, learning to work with her right hand and allowing her art to evolve alongside her changing body.
For Judy, creativity was not a distraction from illness, but a way of engaging with it honestly. She remained deeply connected to people around her and committed to living as fully as possible, even as she faced her reality of a terminal diagnosis.
“She always showed us how to live,” Roy recalls a close friend saying about Judy. “Now she’s showing us how to die.”
Keeping a promise
Judy died in October 2016, after time in hospice that Roy describes as both heartbreaking and deeply meaningful. In his following years, he turned to journaling as a way to survive his abysmal grief.
“For 2 years, I journaled every day,” Roy said. “Sometimes 2 or 3 times a day, whether I was on my porch or in a local pub or a restaurant or the Grand Canyon, you would find me with my journal in hand.”
His writing became a form of self-therapy, a place to hold and process anger, memories, gratitude, and loss all at once. Over time, it also became the foundation for something Judy had asked Roy to do before she died.
“She made me promise to publish her art and her words,” Roy said. “And I said yes, not knowing at the time what that might look like.”
The result was a book built from Judy’s artwork and writing and interwoven with Roy’s journals to become a 3-part story about living well, dying honestly, and finding a way forward. What began as a promise became a project that took 5 years to complete and eventually reached far beyond Roy’s immediate circle. They edited over 950,000 words from him and Judy down to about 85,000 for the book.
Roy is clear that their memoir and award-winning love story was never meant for a narrow audience. It has resonated with people navigating serious illness, caregivers walking alongside loved ones, and healthcare professionals seeking to better understand the lived experience of patients and families.
“I’ve heard from hospice workers, nurses, and social workers who said it helped them better understand the people they care for,” said Roy. Others have told him they read the book not because they were facing illness themselves, but because they wanted to understand who they hoped to be when life becomes difficult for them.
Today, Roy and his new wife, June, give the book, “It All Belongs,” away freely, believing it is meant to be in people’s hands rather than on a warehouse shelf. Copies are available at no cost, with readers asked only to cover shipping. To learn more or request a copy, visit http://itallbelongsbook.com and use code “GO2Cancer” for your free copy.
June

June had been part of Roy’s life long before his lung cancer diagnosis. June met Roy’s late wife Judy through their Ohio church and became close friends. After she died, June and Roy became support for each other, and when Roy learned he had lung cancer, June was one of the first people he called.
“She screamed,” Roy remembered. “And I hated making her feel such pain.”
At that time, June and Roy were just beginning to recognize their growing feelings for each other, but for June, her decision to stay, to support Roy, and eventually to build a life together was instinctive.
“I had this voice that said, ‘I’m not going to let him go through this by himself. He’s already lost his wife of almost 40 years and had more than enough pain from her death,” she said. “I didn’t care where we were going to go or what we had to go through. I was in.”
When Roy proposed, he made sure June understood the reality of his diagnosis. “I said, ‘Do you realize I may not be here in 2 years?” he recalled.
Her answer was immediate. “Well, it’ll be the 2 best years of my life.”
June attended every appointment and every treatment with Roy, and their love deepened even as they navigated all of lung cancer’s difficult challenges together.
They married in Iona, Scotland during Roy’s treatment, after asking his care team whether it was safe to travel. Their answer was yes, and the moment became one of joy woven into a difficult chapter.
What comes next
For more than 5 years after completing treatment, Roy’s scans remained clear. Then, in the fall of 2025 during a routine follow-up appointment with his new oncologist at the Dana-Farber Cancer Institute after a move to Maine, everything shifted again.
“Dr. Sands walked in,” Roy said. “And for the first time he didn’t say, ‘We didn’t find anything.’ Immediately, I knew something was wrong.”
A new tumor had appeared in the same area of his lung that had already been heavily treated. Because of prior radiation and scarring, many treatment options were no longer possible.
“Every option we brought up – radiation, surgery – they just kept getting pushed off the table,” Roy said. “That has been really hard.”
After consultations with multiple specialists, Roy and his care team determined that immunotherapy would likely be their next step. They are currently waiting on additional testing to confirm this as their treatment course, and Roy is eager to get started. While their next steps are currently uncertain, Roy is not without perspective.
“For me to be loved by two such incredible women and to be able to love two incredible women in one lifetime,” he said, “I don’t need a whole lot else. We’ll figure out the rest.”
If you or a loved one are facing similar uncertainty—whether newly diagnosed or navigating what’s next—GO2’s LungMATCH team can help you understand treatment options, including clinical trials, and talk through next steps. Call 1-800-298-2436 or email support@go2.org to connect with a LungMATCH Navigator. to connect with a LungMATCH Navigator.
