Lung cancer support

Find practical advice, emotional support, and resources to help you or your loved one cope with the challenges of living with lung cancer.
Learn about local and national events where you can connect, raise awareness, and support the lung cancer community.
Explore real stories honoring survivors and those remembered through their lasting legacy. Select a category to find stories that resonate most with you.
Find practical advice, emotional support, and resources to help you or your loved one cope with the challenges of living with lung cancer.
Stay informed about the policies that impact the lung cancer community and ways you can get involved.
Explore breakthroughs and ongoing studies in lung cancer research, from clinical trials to cutting-edge therapies and prevention.
Catch up on highlights from our newsletter, featuring stories, resources, and upcoming opportunities to engage.
Explore news and updates shaping the lung cancer landscape—from scientific breakthroughs and organizational milestones to awareness campaigns and community highlights.


May 13, 2026
A diagnosis of small cell lung cancer (SCLC) can bring a wide range of emotions. If you’re feeling uncertain, afraid, or overwhelmed, connecting with others who have faced similar experiences can offer both comfort and strength. Hearing from people who have been living well with SCLC for years is a powerful reminder that your story is still unfolding.
Connection can take many forms, including support groups, one-on-one peer support, or simply reading others’ stories. Each of these forms of connection can help ease feelings of isolation and provide a sense of shared understanding. You are not alone in this. Others are walking this path too, and when asked, here’s what they want you to know.
Take it one step at a time
Focus on today - this appointment, this decision, this moment. Thinking too far ahead can be overwhelming when there is so much unknown in the path ahead. Try to stay in the present and remember that progress isn’t about having everything figured out. It’s about continuing forward one step at a time. There will be good days and hard days. Both are part of the process.
Advocate for yourself
Your healthcare team matters, and you are the most important person on that team. Your thoughts, feelings, and perspectives guide your treatment and care decisions. Your healthcare team should listen and respect you. Whether it’s asking questions, exploring clinical trials, or discussing needs, your voice matters.
- Ask questions until you understand your diagnosis and treatment options.
- Consider getting a second opinion from a thoracic oncologist (lung cancer specialist).
- If something doesn’t feel right, trust your instincts and consider a change.
Let people in (even when it’s hard)
Support can make a huge difference, but accepting help isn’t always easy. The offer of help from friends and family is one way they show their love for you. Accepting their help allows them to be with you through this experience and has the power to strengthen relationships and deepen bonds.
Take care of your body and keep moving
Self-care, even on tough days, can help you both physically and mentally. Even small actions matter.
- Spend time in nature
- Go for a walk when you can
- Eat and hydrate as best you’re able
- Follow your care team’s guidance
- Do something you enjoy
Be honest about how you feel and focus on what you can control
Positivity helps, but it doesn’t mean ignoring fear, frustration, or sadness. It’s okay to feel all of it. What matters is not getting stuck there. Give yourself permission to have hard moments, then try to find your way forward, step by step.
There’s a lot you can’t control with cancer. But there are things you can:
- How you spend your time
- Who you surround yourself with
- How you approach decisions
Some people find strength in learning everything they can. Others focus on daily routines or small goals. There’s no single right way, only what works for you.
Find meaning where you can and hold onto hope
Many people describe a shift in perspective after diagnosis. Time feels different. Priorities become clearer. That means something different for everyone. For you, it could mean:
- Spending more time with loved ones
- Helping others facing cancer
- Finding purpose in advocacy or community
- Setting goals or challenges for yourself and meeting them
Discover what brings you peace, laughter, and enjoyment, and then do more of that.
SCLC is serious. It’s okay to acknowledge that. But hope has a definite place here, not as denial, but as possibility. Treatments are improving. Research is ongoing. And your experience is your own. You don’t have to have everything figured out. You just keep moving forward, one step, one decision, one day at a time.
If you would like to learn more about SCLC, have questions, or need support, our SCLC program can help. Contact our free HelpLine at 1-800-298-2436 or email support@go2.org.


May 5, 2026

For Amita Jain, MD, lung cancer is not just a diagnosis. It’s a lived experience that has shaped her life across multiple roles as a physician, a patient, a daughter, a caregiver, and an advocate.
Her family’s lung cancer story spans generations. In July 2018, her mother, Usha Jain, a retired UC Berkeley professor, was diagnosed with stage 4 (IV) non-small cell lung cancer (NSCLC) despite having no smoking history. Just 6 months later, Amita herself would receive the same diagnosis.
While both women faced advanced disease, their treatment paths diverged. Usha underwent chemotherapy and immunotherapy for nearly 2 years before stopping treatment and transitioning to routine scans. That period (often described clinically as “watch and wait”) felt anything but passive to her family.
“It was hard to feel as though we were ‘doing nothing,’” Amita recalls.
Turning to navigation for answers
As both a physician and a caregiver, Amita understood medicine, but even she found the complexity of lung cancer care overwhelming.
Navigating next steps after treatment, understanding emerging options, and keeping up with rapidly evolving research can feel like a full-time job, especially for families already carrying the emotional weight of a diagnosis.
So, Amita reached out to GO2's LungMATCH navigation program.
“I called the navigators and furnished my mom’s tumor’s genetic profile,” she says. “They reached out a day later with information on some trials for which she might qualify.”
Although her mother ultimately chose not to pursue clinical trials, the impact of that interaction was profound.
“While we did not take action on the options that the navigator provided, the information was empowering,” Amita explains. “It really helped us understand the ‘lay of the land’ in her particular situation.”
Bridging the gap between information and understanding
Even for someone with medical training, the experience revealed an important truth. Access to information is not the same as understanding it.
“Navigating is complex and scary, and getting all the information is difficult if you are not an oncologist,” Amita says. “The navigator that I spoke with was both professional and prompt. That information made me feel as though we understood our options—and that was extremely reassuring.”
For patients and families, that reassurance can be transformative.
A lung cancer diagnosis often brings not only fear, but also a sense of powerlessness. Decisions feel urgent; stakes are high, and the volume of information can be paralyzing.
“The navigator can serve as a bridge to knowledge,” Amita says. “Knowledge is power. Having a diagnosis of lung cancer can be shocking, but more importantly you do feel a bit powerless and overwhelmed. The navigators serve as a resource and lifeline.”
The invisible work of navigation
What many patients don’t see is the depth of work happening behind the scenes.
Navigators are constantly reviewing evolving research, identifying clinical trials, interpreting biomarker data, and translating complex medical information into something patients can actually use to discuss with their care teams.
“Keeping up on the information is a full-time job that most of us are not trained to do,” Amita says.
That expertise becomes especially critical at moments of uncertainty, like when treatment ends, and the path forward is unclear.
In those moments, navigation doesn’t just guide decisions; it restores a sense of control.
Strengthening navigation for the future
Stories like Amita’s mother’s underscore the critical role navigators play, not just in coordinating care, but in empowering patients and families with clarity, confidence, and connection.
To support and strengthen this role, GO2 for Lung Cancer partnered with leading experts to develop a comprehensive resource for those on the front lines of patient care.
The Lung Cancer Navigator: A Guide for Nurses and Allied Health Professionals textbook is designed to equip health professionals with the knowledge and tools they need to guide patients through every step of the lung cancer experience, from diagnosis to survivorship.
By investing in navigator education, we can ensure that more patients and families experience what Amita describes so clearly: the shift from feeling overwhelmed and uncertain to being informed and empowered.

April 14, 2026
Small cell lung cancer (SCLC) is 1 of the 2 main types of lung cancer and accounts for about 15 out of 100 (15%) cases. For decades, treatment for SCLC included chemotherapy, radiation therapy, or surgery if diagnosed in early stages.
It wasn’t until 2018 that the first immunotherapy for SCLC was approved by the Food and Drug Administration (FDA). This was an important advancement in treating SCLC, as immunotherapy works very differently from other treatment types. In October 2025, another breakthrough occurred in the field of immunotherapy when a new type of immunotherapy, a T-cell engager, was approved for SCLC.
These advancements bring hope and optimism to SCLC and expand treatment options. Understanding immunotherapy, how it works, and when it may be used helps you have informed conversations with your healthcare team and stay involved in decision-making. This is important because being knowledgeable allows you to advocate for what matters most to you.
What is immunotherapy?
Your immune system defends your body against germs and diseases that can cause illness. Most of the time, it can tell which cells are healthy and which are not. This enables the immune system to target disease and germ cells without harming healthy cells.
When your immune system detects cancer cells, it goes to work destroying them. Sometimes, it has trouble finding cancer cells because they can appear like healthy cells. Immunotherapy helps your immune system find and attack cancer cells.
Types of immunotherapy
Currently, there are 2 main types of immunotherapies used in SCLC: checkpoint inhibitors and T-cell engagers. They each work in very different ways and are used in different points in treatment.
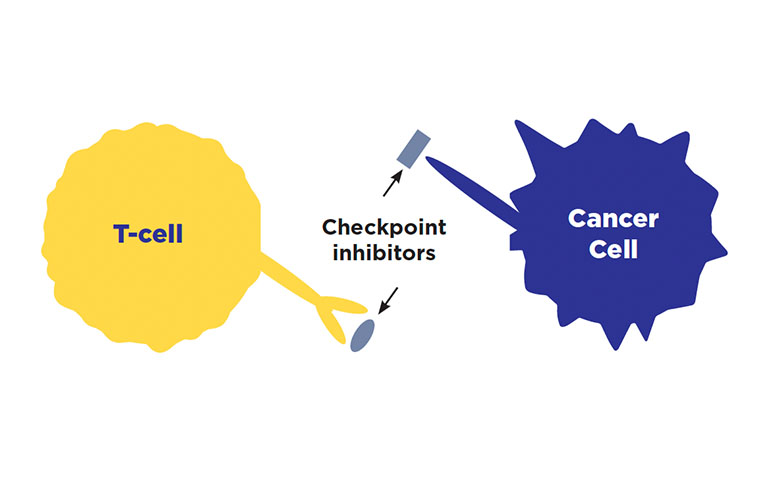
Checkpoint inhibitors
How do they work?
Cancer cells can hide from the immune system by attaching themselves to immune cells. Cancer cells can attach to immune cells at an area called a checkpoint. This sends a signal to your immune system that the cancer cell is healthy, which prevents the immune system cell from attacking it. A checkpoint inhibitor works by blocking cancer cells from attaching to immune system cells, allowing the immune system to better attack the cancer.

When are they used to treat SCLC?
Imfinzi (durvalumab) and Tecentriq (atezolizumab); however, recent clinical trials have broadened their approved uses in different ways.
- Limited-stage SCLC (stages 1, 2, 3): Imfinzi (durvalumab) can be used after chemotherapy and radiation treatments are complete and may be continued for up to 2 years.
- Extensive-stage SCLC (stage 4): Imfinzi (durvalumab) or Tecentriq (atezolizumab) can be used in combination with chemotherapy. Imfinzi may be continued alone after chemotherapy is completed for as long as it is effective and well-tolerated. This is called maintenance therapy. Tecentriq (atezolizumab) may also be used as maintenance therapy either alone or combined with the chemotherapy drug Lurbinectedin.
T-cell engagers
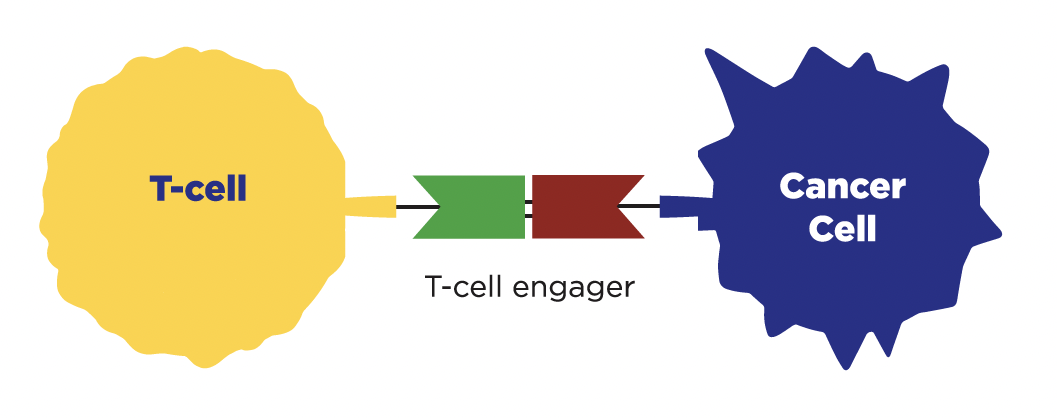
How do they work?
T-cell engagers, such as Imdelltra (tarlatamab), work like a matchmaker. They attach to a T-cell (a type of immune cell that fights germs and diseases) and a cancer cell, bringing them close together. This connection helps your immune system find and attack cancer cells.
When are they used to treat SCLC?
T-cell engagers are FDA-approved for use in extensive-stage SCLC that has spread during or after chemotherapy.
Immunotherapy side effects
The side effects you may experience from immunotherapy will be unique to you. Some common side effects are mild, while others can be more severe. Immunotherapy boosts your immune system's activity, which can sometimes impact healthy cells and organs, leading to inflammation. This requires prompt medical attention.
Ask a member of your healthcare team what common and more serious side effects may occur with your specific type of immunotherapy and know when you should seek immediate medical care.
The future of immunotherapy in SCLC
Immunotherapy is not 1 single treatment; it’s a growing toolbox of therapies. In fact, there are many clinical trials currently underway that focus on:
- Expanding how the currently approved immunotherapies are used to improve outcomes, including using them in earlier stages or combined with other treatments
- Developing new immunotherapy treatments that work differently from the current options
- Exploring ways to boost the body’s immune system and impact the tumor to make it easier to target and attack Questions for your healthcare team
It’s important to talk to your healthcare team about all your treatment options, including immunotherapy. The following questions may be helpful to ask in your conversation:
- Is immunotherapy right for me?
- What side effects should I be aware of with the type of immunotherapy recommended for me?
- Are there any clinical trials that may be right for me?


March 11, 2026
Small cell lung cancer (SCLC) accounts for about 15 out of every 100 (15%) lung cancer cases. After decades of very few changes in the treatment of SCLC, there are now more treatment options, which have shifted the standard of care and bring renewed hope. Whether you’ve just been diagnosed with SCLC or are further down your treatment path, it’s important to know all of your treatment options so you can make informed decisions about your care.
SCLC stages
SCLC treatments are approved for use at different stages of the disease. While many cancers are divided into 4 stages: 1 (I), 2 (II), 3 (III), and 4 (IV) according to the size and location of tumors, SCLC is usually divided into 2 stages.
- Limited-Stage SCLC: Includes stages 1-3 (I-III), when the cancer is on one side of the chest and has not spread very far.
- Extensive-Stage SCLC: Includes stage 4 (IV), when the cancer has spread beyond one side of the chest to other lung areas, lymph nodes, and/or distant organs.
Your specific treatment options will be based on the stage of lung cancer, your previous treatments, the location of lung cancer in the body, and your overall health.
Limited-stage SCLC treatments
In limited-stage SCLC, approved treatments may include one or more of the following:
- Chemotherapy + Radiation: This is the most common treatment for limited-stage SCLC. Giving chemotherapy and radiation at the same time often works better, though you may receive them one after the other, depending on your overall health.
- Chemotherapy kills fast-growing cells in the body, like cancer cells, and is given in repeated cycles, often over several months. Two chemotherapy medicines (etoposide plus either carboplatin or cisplatin) are combined to treat SCLC.
- Radiation therapy (chest radiation) uses high-energy beams to kill or shrink cancer cells or prevent them from spreading.
- Immunotherapy: Checkpoint inhibitors are a type of immunotherapy that activate your immune system to find and fight cancer cells. Imfinzi (durvalumab) is the checkpoint inhibitor approved for use after chemotherapy and radiation are completed if cancer has not spread.
- Surgery: Removing cancer through surgery may be an option if it’s found very early. The surgeon will often also remove and examine nearby lymph nodes to ensure the cancer has not spread.
Extensive-stage SCLC treatments
In extensive-stage SCLC, your first treatment(s) after diagnosis may include 1 or more of the following:
- Chemotherapy: The same chemotherapy drugs used in limited-stage SCLC (etoposide plus carboplatin or cisplatin) may be used as initial treatment for extensive-stage SCLC.
- Immunotherapy: Imfinzi (durvalumab) or Tecentriq (atezolizumab) are the checkpoint inhibitors approved for use during or after chemotherapy is complete.
- Radiation therapy: This treatment may be used to treat areas in the body that didn’t respond to other treatments, or to relieve symptoms. There are also specialized types of radiation used to treat SCLC that has spread to the brain.
If your scans show that the cancer has completely or partially responded to your last round of chemotherapy, or if the cancer is stable and not growing, your healthcare team may discuss starting maintenance therapy. This is the continued use of certain treatments with the goal of keeping cancer from growing. Approved maintenance treatments for extensive-stage SCLC include:
- Immunotherapy: The checkpoint inhibitors, Imfinzi (durvalumab) or Tecentriq (atezolizumab) may be used after chemotherapy is complete as long as they continue to be effective.
- Tecentriq (atezolizumab) combined with Zepzelca (lurbinectedin): Recent studies have shown that Tecentriq (atezolizumab) combined with the chemotherapy drug Zepzelca (lurbinectedin) is more effective as maintenance therapy than Tecentriq (atezolizumab) alone.
Treatment options if SCLC grows or spreads
If your scans show that SCLC has grown or has spread while on your current treatment, a different treatment will be needed. Your healthcare team will talk to you about your options, including well-established treatments, newly approved treatments, and clinical trials. Your options may include one or more of the following:
- Immunotherapy: T-cell engagers are a different type of immunotherapy that work by bringing immune cells together with cancer cells to help activate your immune system and destroy the cancer cells. Imdelltra (tarlatamab) is currently the only approved T-cell engager for SCLC and is the current standard of care when the cancer has grown or spread following chemotherapy.
- Chemotherapy: Your treatment options depend on the type of chemotherapy used previously and how long ago it was. There are several chemotherapy options for SCLC.
- Radiation therapy: There are different types of radiation therapy that may be used to treat specific areas of the body or to relieve symptoms and improve quality of life.
Clinical trials
A clinical trial is a type of research study that tests new treatments or old treatments in new ways to learn how well they work and how safe they are. It’s always a good idea to discuss clinical trials any time a new treatment is needed, including when you are first diagnosed. You can talk to your healthcare team about what clinical trials may be right for you or contact our HelpLine at 1-800-298-2436 or email support@go2.org to connect with our LungMATCH treatment and clinical trial navigators.
Palliative care
Palliative care is different than hospice care. The goal of palliative care is to improve your comfort and your quality of life, no matter the stage of cancer or where you are on your treatment path. Its purpose is to prevent or treat the symptoms and side effects of lung cancer and its treatments so you can enjoy more of life.
Palliative care is especially important in advanced lung cancer. Studies show that people with lung cancer who receive ongoing palliative care beginning early in the treatment process not only have improved quality of life but also live longer.
What does this mean for you?
With ongoing research and recent advances, there is increased hope for people diagnosed with SCLC. New discoveries in SCLC treatment make it even more important to ask your healthcare team about all your available treatment options. Have open discussions with your team about what is important to you and ask questions.
If you would like to learn more about SCLC treatment options, have questions about SCLC, or need support, our SCLC program can help. Contact our free HelpLine at 1-800-298-2436 or email support@go2.org.


February 3, 2026

June & Roy live in Kennebunk, Maine, a place they moved after visiting and vacationing many times throughout their lives. They enjoy barefoot beach walks, snowshoeing, many volunteer activities focused on environmental issues, Indigenous People’s rights, social justice issues, and textile drives organized by June which have kept over 20 tons of textiles and footwear out of landfills. They also enjoy exploring Maine’s forests and mountain areas. June is a retired clinical registered dietician while Roy is a retired banking executive and director. They see a return trip to Switzerland and other excursions in their future. Their favorite toast with an adult beverage is “Ein Sache”, followed by “Uns” — German for “One Thing” and “Us”. Roy is still trying to find where June hid his heart when she stole it. She promises him that it’s in a safe place.
After a history of heart disease, Roy has learned to pay attention to his body, so when he experienced shortness of breath in July 2018, he went to the emergency room. This time, his heart wasn’t his problem. Imaging revealed a large mass in his upper right lung and, with it, a diagnosis that would reshape his years ahead.
Doctors moved quickly. A biopsy confirmed lung cancer, and additional scans showed it had spread to nearby lymph nodes, ruling out surgery. Roy was referred to David Carbone, MD, PhD at The James Comprehensive Cancer Center, where a treatment plan came together quickly.
Roy enrolled in a clinical trial led by Dr. Carbone to explore using immunotherapy in people with stage 3 (III) non-small cell lung cancer (NSCLC). He would receive immunotherapy, then radiation, then chemo, and then immunotherapy again.
The early months were manageable, and Roy didn’t experience any side effects during his initial immunotherapy infusions. Radiation and chemotherapy followed, spaced carefully over many weeks. But toward the end of treatment, a rare and severe reaction to chemotherapy landed Roy in the hospital for 10 days.
This experience forced difficult treatment decisions and required Roy to advocate for himself, something he had learned to do years earlier while caring for his late wife during her illness. Immunotherapy was paused, then ultimately stopped altogether, when Roy developed serious gastrointestinal side effects. By that point, his treatment had already achieved a complete response, and his body could not tolerate continuing.
With treatment complete, Roy entered a new phase: survivorship, including regular monitoring and cautious hope. Follow-up scans initially came every 6 months, then 9, then eventually once a year.
Judy’s story
Roy’s experience with lung cancer was not his first time navigating serious illness. Just a few years earlier, he had walked a parallel path alongside his late wife, Judy.
In November 2015, Judy collapsed in their shower at their home in southeastern Ohio. At the hospital, imaging revealed a large mass in her brain. Judy immediately understood what that meant. Her aunt had died of glioblastoma years earlier, and Judy had been one of her caregivers.
Judy underwent brain surgery the day before Thanksgiving, followed by months of treatment including clinical trials, aggressive chemotherapy, and a 2nd surgery. Despite everything, Roy remembers her determination to keep living fully and authentically, even as options narrowed.
Judy approached her illness with the same intention and creativity that defined her entire life. A spiritual director and artist, she continued creating throughout her treatment, painting, weaving, and writing as a way to make meaning of what she was experiencing. Even after a stroke affected her body’s complete left side (she was left-handed), she adapted, learning to work with her right hand and allowing her art to evolve alongside her changing body.
For Judy, creativity was not a distraction from illness, but a way of engaging with it honestly. She remained deeply connected to people around her and committed to living as fully as possible, even as she faced her reality of a terminal diagnosis.
“She always showed us how to live,” Roy recalls a close friend saying about Judy. “Now she’s showing us how to die.”
Keeping a promise
Judy died in October 2016, after time in hospice that Roy describes as both heartbreaking and deeply meaningful. In his following years, he turned to journaling as a way to survive his abysmal grief.
“For 2 years, I journaled every day,” Roy said. “Sometimes 2 or 3 times a day, whether I was on my porch or in a local pub or a restaurant or the Grand Canyon, you would find me with my journal in hand.”
His writing became a form of self-therapy, a place to hold and process anger, memories, gratitude, and loss all at once. Over time, it also became the foundation for something Judy had asked Roy to do before she died.
“She made me promise to publish her art and her words,” Roy said. “And I said yes, not knowing at the time what that might look like.”
The result was a book built from Judy’s artwork and writing and interwoven with Roy’s journals to become a 3-part story about living well, dying honestly, and finding a way forward. What began as a promise became a project that took 5 years to complete and eventually reached far beyond Roy’s immediate circle. They edited over 950,000 words from him and Judy down to about 85,000 for the book.
Roy is clear that their memoir and award-winning love story was never meant for a narrow audience. It has resonated with people navigating serious illness, caregivers walking alongside loved ones, and healthcare professionals seeking to better understand the lived experience of patients and families.
“I’ve heard from hospice workers, nurses, and social workers who said it helped them better understand the people they care for,” said Roy. Others have told him they read the book not because they were facing illness themselves, but because they wanted to understand who they hoped to be when life becomes difficult for them.
Today, Roy and his new wife, June, give the book, “It All Belongs,” away freely, believing it is meant to be in people’s hands rather than on a warehouse shelf. Copies are available at no cost, with readers asked only to cover shipping. To learn more or request a copy, visit http://itallbelongsbook.com and use code “GO2Cancer” for your free copy.
June

June had been part of Roy’s life long before his lung cancer diagnosis. June met Roy’s late wife Judy through their Ohio church and became close friends. After she died, June and Roy became support for each other, and when Roy learned he had lung cancer, June was one of the first people he called.
“She screamed,” Roy remembered. “And I hated making her feel such pain.”
At that time, June and Roy were just beginning to recognize their growing feelings for each other, but for June, her decision to stay, to support Roy, and eventually to build a life together was instinctive.
“I had this voice that said, ‘I’m not going to let him go through this by himself. He’s already lost his wife of almost 40 years and had more than enough pain from her death,” she said. “I didn’t care where we were going to go or what we had to go through. I was in.”
When Roy proposed, he made sure June understood the reality of his diagnosis. “I said, ‘Do you realize I may not be here in 2 years?” he recalled.
Her answer was immediate. “Well, it’ll be the 2 best years of my life.”
June attended every appointment and every treatment with Roy, and their love deepened even as they navigated all of lung cancer’s difficult challenges together.
They married in Iona, Scotland during Roy’s treatment, after asking his care team whether it was safe to travel. Their answer was yes, and the moment became one of joy woven into a difficult chapter.
What comes next
For more than 5 years after completing treatment, Roy’s scans remained clear. Then, in the fall of 2025 during a routine follow-up appointment with his new oncologist at the Dana-Farber Cancer Institute after a move to Maine, everything shifted again.
“Dr. Sands walked in,” Roy said. “And for the first time he didn’t say, ‘We didn’t find anything.’ Immediately, I knew something was wrong.”
A new tumor had appeared in the same area of his lung that had already been heavily treated. Because of prior radiation and scarring, many treatment options were no longer possible.
“Every option we brought up – radiation, surgery – they just kept getting pushed off the table,” Roy said. “That has been really hard.”
After consultations with multiple specialists, Roy and his care team determined that immunotherapy would likely be their next step. They are currently waiting on additional testing to confirm this as their treatment course, and Roy is eager to get started. While their next steps are currently uncertain, Roy is not without perspective.
“For me to be loved by two such incredible women and to be able to love two incredible women in one lifetime,” he said, “I don’t need a whole lot else. We’ll figure out the rest.”
If you or a loved one are facing similar uncertainty—whether newly diagnosed or navigating what’s next—GO2’s LungMATCH team can help you understand treatment options, including clinical trials, and talk through next steps. Call 1-800-298-2436 or email support@go2.org to connect with a LungMATCH Navigator. to connect with a LungMATCH Navigator.


January 26, 2026
The start of a new year is a great time to take a fresh look at your health insurance. Many insurance benefits reset in January, which means you may have new chances to get care at a lower cost. If you are at risk for lung cancer or living with lung cancer, using your insurance wisely can help you stay healthier and reduce stress.
Here are some tips that can help you make the most of your insurance in the new year.
Know what your insurance covers
Before scheduling appointments, take time to review your health insurance plan. This can help you avoid surprise bills later.
Look for details about:
- Preventive care and screenings
- Doctor visits and specialist visits
- Prescription drug coverage
- Deductibles, copays, and out-of-pocket limits
You can usually find this information on your insurance company’s website or by calling the phone number on your insurance card.
Take advantage of lung cancer screening
If you are at high risk for lung cancer, lung cancer screening could save your life. Most insurance plans, including Medicare, cover annual low-dose CT (LDCT) scans for people who meet certain age and smoking history guidelines. Lung cancer screening:
- Can find lung cancer early, when it is easier to treat
- Is often covered at no cost as preventive care
- Only takes a few minutes
If you think you may qualify, talk to your doctor. Don’t miss out on this important benefit.
Schedule preventive doctor visits early
Many insurance plans cover preventive care visits at no extra cost. These visits help catch health problems early and keep you on track. Consider scheduling:
- An annual primary care check-up
- Follow-up visits if you have symptoms like coughing, shortness of breath, or chest pain
- Smoking cessation counseling if you currently smoke or recently quit
Booking these visits early can help you use your benefits before schedules fill up later in the year.
Understand your specialist coverage
People at risk for lung cancer may need to see specialists, such as:
- Pulmonologists (lung doctors)
- Oncologists (cancer doctors)
- Radiologists (providers who do imaging/screening)
Check whether you need a referral to see a specialist and confirm that the provider is in-network. Staying in-network usually means lower costs for you.
Plan around your deductible
Your deductible is the amount you must pay before insurance starts covering more of your care. Deductibles often reset in January. If you know you’ll need tests, scans, or regular visits:
- Plan care throughout the year to spread out costs
- Ask your provider about estimated costs ahead of time
- Keep track of bills and payments, including receipts
Once you meet your deductible, insurance may cover a larger share of your care.
Use an FSA or HSA to save money on care
A flexible spending account (FSA) or health savings account (HSA) is a special savings account you can use to pay for health care. You put money into the account before taxes are taken out, which helps you save money. You can use these funds to pay for things like doctor visits, scans, prescriptions, and some medical supplies. FSAs usually must be used within the year, while HSAs let you keep and grow your money over time. If your insurance plan offers one of these accounts, it can be a smart way to lower your health care costs.
Review prescription benefits
Medications can be expensive, especially for people managing chronic conditions or cancer-related symptoms. To save money:
- Check your insurance drug list (formulary)
- Ask about generic options
- See if mail-order pharmacies offer lower prices
- Look into patient assistance programs if needed
Your pharmacist or doctor can often help you explore options.
Ask for help when you need it
Health insurance can be confusing, but you don’t have to figure it out alone. Asking questions can help you feel more confident and avoid unexpected costs. Helpful resources include:
- Insurance customer service representatives
- Hospital financial counselors
- Patient navigators or social workers
If you’d like free, one-on-one guidance through lung cancer resources or just want someone to talk to, contact our HelpLine team at 1-800-298-3426 or support@go2.org.
Start the year strong with your health
A new year brings new opportunities—and that includes taking care of your health. By understanding your insurance benefits and using them early, you can take important steps to protect yourself and your loved ones.
Whether it’s scheduling a lung cancer screening, seeing your doctor, or asking questions about coverage, every small step matters.


January 14, 2026
Lung cancer is one of the most common cancers in the United States, with small cell lung cancer (SCLC) making up about 15 out of every 100 (15%) cases. Like many other types of cancer, lung cancer can spread to the brain and start growing there. This is especially common for SCLC. When this happens, it’s called brain metastases or brain mets. It’s not brain cancer; it’s lung cancer that has spread to the brain.
If you have a diagnosis of SCLC, your healthcare team may discuss the risk of brain metastases, ways to manage that risk, and your treatment options if brain mets occur. It’s important to understand all your choices and openly discuss any questions you have with your healthcare team. This helps you gain the information needed to make informed decisions about your care.
Managing your risk of SCLC brain metastases
There are ways you and your healthcare team can manage your risk of developing SCLC brain mets, including:
- Magnetic resonance imaging (MRI) scans
Regularly scheduled MRI scans are the best way to detect brain metastases early, when they are easier to treat. MRI scans use strong magnets to create highly detailed images of the brain. These scans can detect very small changes and are usually scheduled every 3 months. If brain mets are seen on your MRI, your healthcare team will discuss treatment options with you. - MRI scans and prophylactic cranial irradiation (PCI)
Depending on the stage of SCLC you are diagnosed with, your healthcare team may discuss PCI as an option. PCI is a low-dose radiation treatment given to the whole brain to lower the future risk of brain mets. Its goal is to destroy SCLC cells that may be present in the brain, which are too small to detect on MRI scans. PCI is only an option when your brain MRI shows no signs of cancer.
Brain mets can still develop even after PCI treatment, and there are risks of long-term side effects with PCI that can impact memory and other thinking skills. Talk to your healthcare team about the benefits and risks of PCI.
Managing SCLC brain metastases
If your MRI shows brain mets, your healthcare team will discuss your treatment options with you. These options depend on the location and number of metastases, when they are found, your previous treatments, and your overall health and personal goals. Treatment for brain mets can include:
- Whole-brain radiation (WBR) delivers radiation to the whole brain. Typically used when there are many brain metastases.
- Stereotactic radiosurgery (SRS) delivers focused beams of radiation to a specific area of the brain. Used when there is a limited number of brain metastases.
- Immunotherapy helps your immune system to find and destroy cancer cells. Some types of immunotherapy drugs can cross into the brain and destroy cancer cells located there.
- Surgery to remove brain mets may be an option, depending on the location and the number of metastases.
- Clinical trials are research studies done to determine whether a new treatment or combination of treatments is safe and effective. It’s always good to explore clinical trials and discuss your options with your healthcare team. For help finding clinical trials, contact our navigators through our free HelpLine 1-800-298-2436 or email support@go2.org.
Whole brain radiation (WBR) versus prophylactic cranial radiation (PCI)
Sometimes there is confusion between WBR and PCI. While they may sound similar, they are very different and are used for different reasons. Here’s a breakdown in simple terms.
WBR
- When
WBR is given when SCLC has already spread to the brain. - Why
The goal is to treat cancer that is already there. Radiation covers the entire brain to target both visible tumors and cancer cells that may not show up on scans. - What to expect
WBR usually occurs over several treatments, spaced over days or weeks. Common side effects can include fatigue, hair loss, memory or thinking changes, and skin irritation.
PCI
- When
PCI is given when scans do not detect cancer in the brain. It aims to prevent lung cancer from spreading there. PCI’s goal is to destroy SCLC cells that are too small to be seen on an MRI. - Why
The goal is prevention. By treating the whole brain early, PCI can lower the risk of lung cancer spreading to the brain. - What to expect
PCI is usually given in smaller total doses than WBR. Common side effects can be similar, such as fatigue and changes in memory and thinking skills.
The key difference
- WBR = treatment for brain metastases that already exist
- PCI = prevention, used before metastases appear, low-dose radiation
Summary
Understanding how SCLC can affect the brain and the ways to manage your brain health can help you feel more prepared and confident in your care. Having regular MRI scans and thoughtful discussions with your healthcare team about what is important to you in your care can result in an approach to managing SCLC that is just right for you.
If you’d like to learn more about SCLC, have questions, or need support, please contact our free HelpLine at 1-800-298-2436 or email support@go2.org.


December 4, 2025

The holiday season can bring moments of connection, reflection, and comfort—especially for someone navigating a lung cancer diagnosis. Thoughtful, practical gestures can remind someone that they’re not facing challenges alone.
If you’re looking for meaningful ways to show support this season, here are 5 heartfelt gift ideas that center on warmth, self-care, and positivity.
- A soft blanket or cozy socks
Comfort matters, especially on days filled with appointments, treatments, or much-needed rest. A cozy blanket or pair of fuzzy socks can offer a small moment of warmth and security. It’s a simple, everyday reminder that you’re thinking of them. - A nourishing meal
A ready-to-heat meal can be one of the most helpful gifts for people going through treatment and their caregivers. On busy days—or days when energy is low—having something nourishing already prepared can relieve stress and support well-being. - A handwritten card or note of encouragement
Sometimes the most powerful gift is words of support or encouragement. A handwritten card can remind someone that they are not alone. Whether you share a favorite memory or simply let them know you’re here for whatever they need, heartfelt words go a long way. - An uplifting book or journal
Stories can be grounding during long days of rest or treatment. Consider an uplifting read or a journal that gives them space to process their thoughts. If reading feels tiring, an audiobook subscription or a playlist of calming music can be a comforting alternative. - A practical care package
A personalized care bundle can be both thoughtful and useful. Items like lip balm, unscented lotion, herbal tea, a soft hat, or a soothing eye mask can ease everyday discomforts. Tailor it to what you know they’ll appreciate most.
At the heart of each of these gifts is the reminder that someone cares. Whether you offer a warm meal, a handwritten note, or a cozy blanket, the most meaningful message you’re giving is simply you’re not alone.
If you or a loved one have questions or need general support, GO2’s HelpLine is a free, one-on-one service that connects patients and caregivers with experienced staff who can provide guidance, resources, and, most importantly, hope. Call 1-800-298-2436 or email support@go2.org to get started.


December 1, 2025

The lung cancer community is mourning the loss of Bonnie J. Addario, who passed away on August 25, 2025, at the age of 77. She leaves behind her beloved husband of over 40 years, Tony; her children Danielle, Jared, and Andrea; 9 grandchildren; and 5 great-grandchildren—each of whom she nurtured with boundless joy, humor, and unconditional love.
She was a co-founder and leader of GO2 for Lung Cancer, founder of the Bonnie J. Addario Lung Cancer Foundation (ALCF), and co-founder of the Addario Lung Cancer Medical Institute (ALMCI).
When diagnosis becomes purpose
In October 2003, Bonnie received a stage 3B (IIIB) lung cancer diagnosis, transforming her life forever. Facing grim odds, she did not retreat. Instead, she assembled a multidisciplinary medical team—a thoracic surgeon, oncologists, pulmonologists, radiation specialists—to carve out a survival plan.
“If I am going to die from this disease, I don’t want it to be because I did nothing,” she later declared.
Her personal experience ignited a mission: to ensure others would not walk that path alone. With the same fierce compassion she carried into every part of her life, Bonnie founded ALCF in March 2006, proclaiming, “Enough is enough!”
Building on her vision for patient-centered care, Bonnie co-founded GO2 for Lung Cancer, which formed through the merger of ALCF and Lung Cancer Alliance. Through GO2, she worked to ensure that the voices of patients, survivors, caregivers, and advocates were heard, while fostering collaboration with researchers, industry, and public health leaders. Her approach was guided by a “community-centric” philosophy to support the lung cancer community.
From personal experience to patient advocacy
Bonnie’s story began well before her advocacy work. She was a gifted businesswoman who shattered barriers in industries historically dominated by men. As President of Olympian Oil and Commercial Fueling Network (CFN), she led with vision, grace, and tenacity, earning admiration for her leadership and innovation. The resilience and strategic thinking she honed in business would soon become invaluable in facing one of life’s greatest challenges.

For Bonnie, everything began and ended with patients. She knew lung cancer was not just a medical condition but a deeply human one, and she was determined to make sure no one ever felt alone. Her vision was both simple and revolutionary: put patients at the center of every decision, every discovery, and every conversation.
She built a roadmap where none existed, pioneering resources that empowered patients and families to navigate the unknown: a patient education handbook, a shared data registry, and one-on-one counseling to provide both information and direct support.
Perhaps nothing embodies her vision more than the Lung Cancer Living Room®, the education and support series she launched in 2009. What began as a gathering in her own home has since grown into a global lifeline, reaching over a million people in 144 countries. In the Living Room, people diagnosed with lung cancer and families could engage face-to-face—or screen-to-screen—with leading experts, walk away with knowledge, and, more importantly, hope.
Bonnie’s unwavering belief in respect, clarity, and partnership transformed lung cancer care. She built spaces where people could find connection, courage, and the confidence to advocate for themselves. She reminded people that even in the most challenging moments, tomorrow could hold possibilities.
Research that listens: ALCMI
Realizing that patient empowerment needed to be paired with cutting-edge research, Bonnie co-founded the Addario Lung Cancer Medical Institute (ALCMI) in 2008, an international research consortium committed to unlocking lung cancer’s genetic mysteries and advancing targeted treatments.
Breaking down traditional silos, ALCMI brought together more than 25 world-class research institutions into a single collaborative network—something that had never been done before in lung cancer research. The institute established one of the first global lung cancer biobanks, giving scientists and clinicians shared access to patient samples and data to speed discovery. Among its landmark initiatives is the INHERIT study, which identified the first-ever genetic marker linked to increased hereditary risk for lung cancer. Other ALCMI studies have shed light on unique genetic drivers of the disease, improved understanding of young lung cancer, and opened the door to new approaches in targeted therapy and clinical trial design.
By integrating patient perspectives with rigorous scientific investigation, ALCMI continues to accelerate discoveries, improve access to personalized therapies, and create a more precise understanding of the disease. Through this work, Bonnie ensured that research would not remain confined to the laboratory but would translate into tangible benefits for patients, bridging the gap between innovation and care.
Voices that matter: patient stories and youth advocacy

Bonnie believed deeply in the power of stories to drive change. She amplified the voices of people living with lung cancer, ensuring their experiences informed not only support services but also research, policy, and public awareness.
When Bonnie met 21-year-old athlete Jill Costello, she was profoundly moved. Jill’s courage and determination sparked Jill’s Legacy, a youth-focused advocacy group that reminded the world that lung cancer can—and does—impact anyone. This effort inspired a new generation to step forward, raise awareness, and push for progress.
Bonnie also championed groundbreaking research, most notably the Genomics of Young Lung Cancer (GoYLC) study, which identified a previously unknown and unique form of lung cancer in young adults. This was a discovery that had never been recognized before and opened an entirely new area of research. Its follow-up study, Epidemiology of Young Lung Cancer (EoYLC), sought to understand why these otherwise healthy young adults develop the disease by examining environmental, behavioral, and genetic risk factors. This novel, groundbreaking work would not have happened without Bonnie’s vision and determination. Today, findings from these studies are shaping efforts to improve prevention, detection, and treatment—critical steps that will save lives and bring hope to future generations.
Honoring excellence: The Bonnie J. Addario Lectureship Award
Bonnie’s legacy is also carried forward through the Bonnie J. Addario Lectureship Award, established in 2008 to honor individuals whose work profoundly influenced lung cancer research, education, and patient advocacy.
Each recipient joins an esteemed group of pioneers whose contributions mirror Bonnie’s insistence on pushing boundaries, asking the hard questions, and never accepting the status quo. The Lectureship Award ensures that her spirit of courage, urgency, and hope continues to inspire the people who shape the future of lung cancer care.
Championing precision care: biomarker testing
Bonnie was a founding voice in urging patients and the medical community to embrace comprehensive biomarker testing at diagnosis and progression. She emphasized that lung cancer is not one singular disease and when biomarkers are identified, doors open to targeted therapies.
In November 2023, she received the prestigious Leadership in Personalized Medicine award from the Precision Medicine Coalition (PMC) for her outstanding impact on lung cancer. Reflecting on the award, Bonnie said:
“It has always been my number one priority to make sure that people with lung cancer feel represented in every conversation and every decision we’ve made at GO2 and certainly in our partnerships with industry and medical institutions. That’s always been a responsibility I’ve taken seriously, but it has also been such an honor to work with so many wonderful people with lung cancer and share their stories and their needs in a way that increases awareness, builds momentum, and improves their lives.”
Final reflection: hope in action

Bonnie’s passing on August 25, 2025, marks the end of a chapter—but her story is far from over. Her legacy lives on in the empowered patients who advocate for themselves, the researchers who continue forging life-saving discoveries, and the countless communities that have found hope through her efforts. Bonnie has made an impact on everyone who has met her and received one of her trademark hugs.
If you’ve been touched by her work, a support session, a resource, a reminder of your own strength—carry forward her spirit. Whether through volunteering, donating, advocating for the lung cancer community, or simply sharing her story, you can help ensure Bonnie’s greatest gift—hope—is never forgotten.
To honor Bonnie’s memory, GO2 for Lung Cancer has created the GO2 Bonnie J. Addario Legacy Award that recognizes individuals who embody Bonnie’s unwavering spirit, courageous leadership, and relentless determination to transform the landscape of lung cancer. The 2025 recipients of the award, the Young Lung Cancer Initiative Co-Founders Bianca Bye and Leah Phillips, were honored for empowering and connecting young adults affected by lung cancer.
As a tribute to Bonnie’s extraordinary life and legacy, a group of generous donors has come together to MATCH all gifts 100% through December 31. Your support of the Bonnie J. Addario Legacy Fund will help sustain the patient-centered programs, research, and care she built—and keep hope alive for every person facing lung cancer. Learn more and make a gift here.
