Legacy

Find practical advice, emotional support, and resources to help you or your loved one cope with the challenges of living with lung cancer.


May 6, 2026

For Janaki and Harsha, their wedding wasn’t just about celebrating a new chapter together; it was also an opportunity to honor the past, give back, and make a meaningful impact for others facing lung cancer.
Janaki’s connection to lung cancer is deeply personal. Her late husband, Kartik, was diagnosed with stage 4 (IV) lung cancer at just 28 years old while he was still a third-year internal medicine resident. Through a targeted clinical trial for his EML4/ALK mutation, he was able to continue working for several years before passing in 2015 at the age of 34. His journey continues to inspire Janaki’s commitment to supporting others impacted by the disease.
This was a second marriage that brought together 2 families, not starting from scratch. Material gifts didn’t feel necessary, but they knew their loved ones would still want to give something. That’s when they decided to turn their wedding into a fundraiser in honor of Kartik. “Many of our friends and family were familiar with Kartik’s journey,” Janaki said. “They were more than happy to donate, and several told us they thought it was a great idea.”
Lessons learned along the way
While their fundraiser was a success, Janaki reflects on what she might do differently.
“We didn’t initially go through GO2 because we were trying to get donations matched through companies,” she explained. “But in retrospect, it would have been easier, and likely more effective, to set up a GO2 fundraising page and link it directly on our wedding website.”
Planning ahead, she noted, could have streamlined the process and avoided fees from other fundraising platforms.
But what surprised them most was the incredible generosity of their community. “We were amazed by how much money we were able to raise.”

Tips for turning your own wedding into a fundraiser
For couples considering a similar approach, Janaki offers practical advice:
- Start early. Wedding planning gets busy, so give yourself time to set things up properly.
- Keep it simple. A direct link to a fundraising page makes it easy for guests to contribute.
- Spread the word beyond the website. Share your fundraiser at pre-wedding events or gatherings. Many guests won’t check every page on a website.
- Create in-person opportunities. If you’re hosting events leading up to the wedding, like bridal showers, engagement parties, etc, consider setting up a donation box.
- Ask for help. Friends and family are often eager to support both your wedding and your cause.
Continuing the impact
Even beyond their fundraiser, Janaki continues to connect others to GO2’s resources and recently referred a family friend for support.
“I love seeing what the organization is doing for patients and in research,” she said. “It’s providing hope and that’s one of the most important things when facing lung cancer.”
Make your celebration count
Inspired by Janaki and Harsha’s story? You can turn your own milestone—whether it’s a wedding, birthday, or special event—into a powerful way to support people impacted by lung cancer.
Start your own fundraiser benefiting GO2 and help bring hope to patients and families who need it most.
Learn more about how you can create your own fundraiser for GO2 for Lung Cancer.


December 1, 2025

The lung cancer community is mourning the loss of Bonnie J. Addario, who passed away on August 25, 2025, at the age of 77. She leaves behind her beloved husband of over 40 years, Tony; her children Danielle, Jared, and Andrea; 9 grandchildren; and 5 great-grandchildren—each of whom she nurtured with boundless joy, humor, and unconditional love.
She was a co-founder and leader of GO2 for Lung Cancer, founder of the Bonnie J. Addario Lung Cancer Foundation (ALCF), and co-founder of the Addario Lung Cancer Medical Institute (ALMCI).
When diagnosis becomes purpose
In October 2003, Bonnie received a stage 3B (IIIB) lung cancer diagnosis, transforming her life forever. Facing grim odds, she did not retreat. Instead, she assembled a multidisciplinary medical team—a thoracic surgeon, oncologists, pulmonologists, radiation specialists—to carve out a survival plan.
“If I am going to die from this disease, I don’t want it to be because I did nothing,” she later declared.
Her personal experience ignited a mission: to ensure others would not walk that path alone. With the same fierce compassion she carried into every part of her life, Bonnie founded ALCF in March 2006, proclaiming, “Enough is enough!”
Building on her vision for patient-centered care, Bonnie co-founded GO2 for Lung Cancer, which formed through the merger of ALCF and Lung Cancer Alliance. Through GO2, she worked to ensure that the voices of patients, survivors, caregivers, and advocates were heard, while fostering collaboration with researchers, industry, and public health leaders. Her approach was guided by a “community-centric” philosophy to support the lung cancer community.
From personal experience to patient advocacy
Bonnie’s story began well before her advocacy work. She was a gifted businesswoman who shattered barriers in industries historically dominated by men. As President of Olympian Oil and Commercial Fueling Network (CFN), she led with vision, grace, and tenacity, earning admiration for her leadership and innovation. The resilience and strategic thinking she honed in business would soon become invaluable in facing one of life’s greatest challenges.

For Bonnie, everything began and ended with patients. She knew lung cancer was not just a medical condition but a deeply human one, and she was determined to make sure no one ever felt alone. Her vision was both simple and revolutionary: put patients at the center of every decision, every discovery, and every conversation.
She built a roadmap where none existed, pioneering resources that empowered patients and families to navigate the unknown: a patient education handbook, a shared data registry, and one-on-one counseling to provide both information and direct support.
Perhaps nothing embodies her vision more than the Lung Cancer Living Room®, the education and support series she launched in 2009. What began as a gathering in her own home has since grown into a global lifeline, reaching over a million people in 144 countries. In the Living Room, people diagnosed with lung cancer and families could engage face-to-face—or screen-to-screen—with leading experts, walk away with knowledge, and, more importantly, hope.
Bonnie’s unwavering belief in respect, clarity, and partnership transformed lung cancer care. She built spaces where people could find connection, courage, and the confidence to advocate for themselves. She reminded people that even in the most challenging moments, tomorrow could hold possibilities.
Research that listens: ALCMI
Realizing that patient empowerment needed to be paired with cutting-edge research, Bonnie co-founded the Addario Lung Cancer Medical Institute (ALCMI) in 2008, an international research consortium committed to unlocking lung cancer’s genetic mysteries and advancing targeted treatments.
Breaking down traditional silos, ALCMI brought together more than 25 world-class research institutions into a single collaborative network—something that had never been done before in lung cancer research. The institute established one of the first global lung cancer biobanks, giving scientists and clinicians shared access to patient samples and data to speed discovery. Among its landmark initiatives is the INHERIT study, which identified the first-ever genetic marker linked to increased hereditary risk for lung cancer. Other ALCMI studies have shed light on unique genetic drivers of the disease, improved understanding of young lung cancer, and opened the door to new approaches in targeted therapy and clinical trial design.
By integrating patient perspectives with rigorous scientific investigation, ALCMI continues to accelerate discoveries, improve access to personalized therapies, and create a more precise understanding of the disease. Through this work, Bonnie ensured that research would not remain confined to the laboratory but would translate into tangible benefits for patients, bridging the gap between innovation and care.
Voices that matter: patient stories and youth advocacy

Bonnie believed deeply in the power of stories to drive change. She amplified the voices of people living with lung cancer, ensuring their experiences informed not only support services but also research, policy, and public awareness.
When Bonnie met 21-year-old athlete Jill Costello, she was profoundly moved. Jill’s courage and determination sparked Jill’s Legacy, a youth-focused advocacy group that reminded the world that lung cancer can—and does—impact anyone. This effort inspired a new generation to step forward, raise awareness, and push for progress.
Bonnie also championed groundbreaking research, most notably the Genomics of Young Lung Cancer (GoYLC) study, which identified a previously unknown and unique form of lung cancer in young adults. This was a discovery that had never been recognized before and opened an entirely new area of research. Its follow-up study, Epidemiology of Young Lung Cancer (EoYLC), sought to understand why these otherwise healthy young adults develop the disease by examining environmental, behavioral, and genetic risk factors. This novel, groundbreaking work would not have happened without Bonnie’s vision and determination. Today, findings from these studies are shaping efforts to improve prevention, detection, and treatment—critical steps that will save lives and bring hope to future generations.
Honoring excellence: The Bonnie J. Addario Lectureship Award
Bonnie’s legacy is also carried forward through the Bonnie J. Addario Lectureship Award, established in 2008 to honor individuals whose work profoundly influenced lung cancer research, education, and patient advocacy.
Each recipient joins an esteemed group of pioneers whose contributions mirror Bonnie’s insistence on pushing boundaries, asking the hard questions, and never accepting the status quo. The Lectureship Award ensures that her spirit of courage, urgency, and hope continues to inspire the people who shape the future of lung cancer care.
Championing precision care: biomarker testing
Bonnie was a founding voice in urging patients and the medical community to embrace comprehensive biomarker testing at diagnosis and progression. She emphasized that lung cancer is not one singular disease and when biomarkers are identified, doors open to targeted therapies.
In November 2023, she received the prestigious Leadership in Personalized Medicine award from the Precision Medicine Coalition (PMC) for her outstanding impact on lung cancer. Reflecting on the award, Bonnie said:
“It has always been my number one priority to make sure that people with lung cancer feel represented in every conversation and every decision we’ve made at GO2 and certainly in our partnerships with industry and medical institutions. That’s always been a responsibility I’ve taken seriously, but it has also been such an honor to work with so many wonderful people with lung cancer and share their stories and their needs in a way that increases awareness, builds momentum, and improves their lives.”
Final reflection: hope in action

Bonnie’s passing on August 25, 2025, marks the end of a chapter—but her story is far from over. Her legacy lives on in the empowered patients who advocate for themselves, the researchers who continue forging life-saving discoveries, and the countless communities that have found hope through her efforts. Bonnie has made an impact on everyone who has met her and received one of her trademark hugs.
If you’ve been touched by her work, a support session, a resource, a reminder of your own strength—carry forward her spirit. Whether through volunteering, donating, advocating for the lung cancer community, or simply sharing her story, you can help ensure Bonnie’s greatest gift—hope—is never forgotten.
To honor Bonnie’s memory, GO2 for Lung Cancer has created the GO2 Bonnie J. Addario Legacy Award that recognizes individuals who embody Bonnie’s unwavering spirit, courageous leadership, and relentless determination to transform the landscape of lung cancer. The 2025 recipients of the award, the Young Lung Cancer Initiative Co-Founders Bianca Bye and Leah Phillips, were honored for empowering and connecting young adults affected by lung cancer.
As a tribute to Bonnie’s extraordinary life and legacy, a group of generous donors has come together to MATCH all gifts 100% through December 31. Your support of the Bonnie J. Addario Legacy Fund will help sustain the patient-centered programs, research, and care she built—and keep hope alive for every person facing lung cancer. Learn more and make a gift here.


September 23, 2024
When Presley Anderson was diagnosed with stage 4 (IV) non-small cell lung cancer (NSCLC) 2 years ago, she immediately wondered what this would mean for her young family. She feared she might not be around to watch her 4 children grow up. A biopsy revealed that her lung cancer has the EGFR mutation, which allows her to take targeted therapy. This treatment, which Presley calls a miracle drug, has been effective in treating her cancer and has put her cancer into remission. Research progress and the development of new treatment options have given Presley hope for the future. Hear more from Presley about her story and the advice she gives to those living with lung cancer.


February 12, 2024
Aundrea H. is a married mother of three who lives in Washington state, where she homeschools her children (ages 17, 15, and 12). She enjoys spending time with her family and friends as well as being involved in church activities.
My diagnosis
In December 2023, I was recovering from a cold and had a cough that kept lingering. I noticed that it was a little difficult to take a deep breath, and there was a wheezing or whistling sound that I’d never heard before. I’m known to put off seeing the doctor, but I decided to call anyway and was surprisingly able to get in for the last opening of the day. My doctor first ordered a chest x-ray and later, a chest CT scan which confirmed there was a mass in my left lung. This was not at all the news I expected. I tried to call my husband at work and couldn’t reach him. My husband is a member of the S.W.A.T. team, and when I called him at work about my scan results, I learned that he was in the middle of an active shooter situation. I couldn’t conceive how both of these highly stressful and emotional situations could be happening to us at the same time. Thankfully, my husband was unharmed in that incident. We would later learn that this event would give him time off that he would otherwise not have had so he could be with me when I needed him most. The evening that I was diagnosed with lung cancer, I spoke with one of my husband’s colleagues who works in the emergency department of our local hospital. He arranged for me to see a pulmonologist the very next day, Dec. 30, 2023. I received a biopsy, and three days later, it confirmed that I had extensive stage small cell lung cancer (SCLC). I was only 37 years old and have never smoked.
My treatment and clinical trial
I started my treatment right away and went through four rounds of chemotherapy with immunotherapy. My repeat scans showed good news–the cancer had shrunk! However, I was told that more treatment was needed to fight the cancer that remained. I understood that my treatment options were limited, and I felt like a clinical trial would be the best way to beat this. My oncologist was able to find a trial that had just opened, and I was going to be the first person to join! I honestly felt so excited to be on the cutting edge of a possible new treatment that could make a difference in my life and the lives of others. Before starting the trial there were moments when I felt nervous, but I also felt strongly that this was the best treatment decision for me. I began the clinical trial three weeks after I finished my fourth and final round of chemotherapy and immunotherapy. Since starting the clinical trial, I’ve had two more scans to monitor my progress. My first scan showed the cancer had continued to shrink, and my most recent scan showed no cancer at all! My doctor says I’m now in remission.
My children
My husband and I found that it was best to be open and honest with our children about all that was happening. We processed everything with them and kept the lines of communication open. We took a break from our homeschooling to focus on my treatment, and we gave them the choice of whether to visit me while I was being monitored in the hospital during the clinical trial. They chose not to come, and that was okay with me because imagining me in the hospital was frightening to them. We have a strong faith in God, and we all rely on that to get us through.
My perspective
I’m eternally grateful for the precise timing and numerous pieces that fit together, leading me to where I am today. My faith is the biggest thing that has kept us all going. Even when things got very difficult, I could see God’s hand in the details. Recognizing even the smallest connections continues to bring me hope. I’m still in the clinical trial and will receive treatment every month for the next two years, as long as there are no complications. I generally feel really good and am not dealing with any real side effects. I would encourage people to be open to learning about and consider joining a clinical trial. The care I received throughout the trial was excellent. I was closely monitored and had regular bloodwork and scans. It feels great to play a part in getting a new treatment out to other people.


November 15, 2023

When Cliff Norton walks into a room, he brings hope through the door with him. Diagnosed with stage 4 (IV) lung cancer in July 2010, he was declared NED (no evidence of disease) in December 2012. More than a decade and many PET scans later, he’s still cancer-free. His story brings hope to others diagnosed with the disease. “People who are newly diagnosed want to talk to, look in the eyes, touch, and hold hands with survivors,” said Norton. “It’s a critical element of having hope.” He knows because he’s been there. Norton’s oncologist introduced him to GO2 for Lung Cancer about six months after his diagnosis. He quickly began to learn more about the disease—and the need for additional education, awareness, and advocacy. That led him to attend his first Lung Cancer Voices Summit. “I was battling lung cancer and I wanted to be with other people who were dealing with the same things I was,” he said. “We’re common souls.” That first summit hooked him in, and he’s been a lung cancer advocate ever since. Today, Norton sits on the Voices Summit Planning & Advisory Committee. Comprised of people living with lung cancer and caregivers, the committee helps develop the event’s agenda to ensure it meets the needs of the lung cancer advocacy community. He’s also held sessions for first-time summit participants on what to expect.
Four bullet points, five minutes

“Going up to Capitol Hill has an impact, especially when we use our time wisely,” said Norton. That’s another reason he encourages people to get involved and attend the Voices Summit. And, of course, he has advice for first-time advocates to maximize their impact. Call it the “four bullets, five minutes” rule. “If we ramble, we waste everyone’s time. So, I tell people to come with four bullets about your story, practice it, rehearse it, and compress it to five minutes,” he said. “Make it personal but be professional as well. That shows you value legislators’ time, and it gives everyone in the group an opportunity to tell their story.” Finally, Norton points out that advocacy does make a difference. “We see impact from it,” he said. “We’re seeing research helping to increase survivorship. When I was diagnosed, they were looking for two genetic mutations in lung cancer; we’re looking for a dozen now. That’s the effect of research. And that’s the effect of going up to Capitol Hill, meeting with your elected officials, telling your story, and having an impact on them so that you encourage them to fund the legislation that's going to make a difference.”


August 29, 2023

My name is Presley and I was diagnosed with stage 4 (IV) non-small cell lung cancer on Sept. 19, 2022. It felt like the rug had been pulled out from under me. I was only 34 years old, a wife, and a mother of four children all under the age of seven at the time. My symptoms were subtle and I would have never known they were related to lung cancer. I never felt sick, nor looked sick. My first symptom was an irregular menstrual cycle so I went to the OB/GYN who ran blood work, all of which came back normal. Because on the outside I appeared to be a healthy mother she dismissed me, brushed off my feelings of fatigue and irregular menses, and pinned it on exhaustion from motherhood. I had been tired for a long time and it turned out there was a greater reason why. Just a few weeks later I was on the floor changing my youngest son's diaper, and decided to do some light stretching. That’s when I heard crunch! Something in my back locked up, leaving me immobilized on the floor for an hour and a half. I was moving some boxes the day before and thought that was the cause. My background in athletics told me to push through and the pain would subside. Fast forward two months later, a couple days after my son’s second birthday and I literally could not get off the couch due to the back pain. I told my husband, “You need to take me to the emergency room or I am going by ambulance.” The doctors at the ER gave me some medication to get back on my feet and referred me for an MRI. Everyone assumed it was a bulging or herniated disc because I looked healthy and did not feel “sick.” Cancer was NOWHERE on the radar. Little did I know my life was about to change forever. We were still in the car driving home from the MRI and “DING!” an email came through – the results were in. It was traumatizing to get results via email for something so significant that I knew nothing about. Before my diagnosis, I didn't even know what an “oncologist” was; learning cancer lingo is like learning a whole new language. The results read, “Suspected widespread skeletal metastases. Moderate pathologic compression fracture of T8. Mass versus consolidation of the right upper lobe. Possible military lung nodules. Dedicated chest CT is recommended.” WHAT?! I was frantic, googling each of those words. I was filled with fear and just plain lost. The CT scan confirmed masses in my lungs, ovary, and liver along with lesions throughout my skeleton including the spine, ribs, scapula, and humerus. Next up was a biopsy of my spine, a PET scan, and an MRI of my brain. The biopsy and PET scan both confirmed malignancy - it felt like my world had been flipped upside down. A few days later I learned the cancer had also spread to my brain. The biopsy showed adenocarcinoma favoring lung primary, however, since there was a mass on my ovary they were still distinguishing if it was lung or ovarian cancer. That same week the radiation oncologist called me and indicated that they were very concerned I may break my hip because the tissue damage from the cancer in my humerus was profound. Radiation to my hip and spine was recommended right away. The next day I sat in her office and asked a simple question, “Is the cancer in my lymph nodes?” “What do you mean in your lymph nodes?” she asked. “Well, I have heard that cancer is really bad if it is in your lymph nodes,” I replied. I will never forget her cold and stoic response. “It’s everywhere. This is stage 4 (IV) lung cancer.” Not only was this the first time I officially heard it was lung cancer, but it also was at the most advanced stage. I shut down and really couldn’t speak after that. The fear was immobilizing and it felt like I had just received a death sentence. She went on to tell me that there was no cure and that the radiation would act like a Band-Aid, only improving my quality of life. I came home that day and laid on the couch. I couldn’t open my eyes and face the reality of what I just learned. Every time I looked at my children I wanted to cry thinking about all of the graduations, weddings, and grandchildren I’d miss. That evening before bed I got down on my knees and prayed for better care. The next day my prayer was answered when I received a call scheduling me for an appointment at MD Anderson Cancer Center with a thoracic oncologist. Without hesitation, my mother and I booked flights to Houston.

This is my favorite part of my story because it is when I gained HOPE! Upon arrival at the cancer center, I felt a sense of ease, I knew I was in the best hands in the country. Not only did each and every nurse and doctor take their time while talking with me, but for the first time a physician laid hands on me! Yes, this was the first time someone gave me a physical exam and listened to my heart and lungs. We did a liquid biopsy test to find out if I had any mutations and it came back EGFR positive. This was the best news! I could take targeted therapy, which is a sophisticated drug that can essentially “turn off” the mutation. I take an oral pill each day that precisely kills and attacks cancer cells only. Many call this medicine a miracle drug because it does exactly that – miraculously just after four months of taking my medication my scan was cancer-free!In November of 2023, my scan showed a slight progression - (3 mm) to my primary tumor in my right upper lung. Radiation was performed at UC Davis by Dr. Daly. I will know more at my next scan in late March. During radiation, I have continued my targeted therapy, and I will likely be on the drug for life. The worst side effect I had from the drug was fatigue. I have to listen to my body and rest more often than I would like to some days.Healing from the inside out has become almost a full-time job. I have vowed to put all my effort into sustaining my remission. I also believe the alternative therapies I have added to my healing journey have helped me get to “NED” – no evidence of disease. If I were to speak with someone just being diagnosed I would tell them the following:
- Get your biomarkers tested ASAP.
- Read, read, and read! But STAY OFF GOOGLE! Make sure you’re reading valid medical research.
- Know that there is HOPE, a positive mindset goes a long way.
- Eat more plants.
- Take charge of your care team, find doctors, and healers that suit you.
- If you have children, hire a Child Life Specialist to help explain your diagnosis in kid-friendly terms.
- Reach out to GO2 for Lung Cancer - they can link you with fellow survivors.


July 13, 2023
By Shelly Engfer-Triebenbach

I was just finishing up my 18th year of teaching music when I noticed myself getting short of breath doing easy things. I went to see my primary care doctor who gave me antibiotics and an inhaler so I could treat what they thought was “pneumonia.” I went back the next day because it felt like my breathing had worsened. A pulmonologist ordered a chest X-ray and then sent me to have a heart echocardiogram which confirmed that I had extra fluid around my heart. I had a pericardiocentesis in which 1.5 liters of fluid was drained from what is called the pericardial sac around my heart, and almost immediately I had an easier time breathing and felt better. The next week I had a follow up appointment with a cardiologist. I was told that they found malignant cells (cancer cells) in the fluid from around my heart. I remember praying so hard for breast cancer because I knew the chances of survival were good and that it was a well-researched cancer. Many tests and several days later, I was told I had stage 4 non-small cell lung cancer. I was shocked and in disbelief. How could I have lung cancer? After all, I didn’t smoke!
The value of second opinions and biomarker testing
The tumor was in the upper right lobe of my lung so I had to have a needle-guided biopsy. The tissue was tested for two biomarkers, ALK and EFGR. If my results showed I had one of these biomarkers, I could have targeted therapy instead of chemotherapy. Both came back negative. Devastated, I started chemotherapy the next week, but I was not settled with my diagnosis. I sought out four second opinions. At the fourth, the oncologist wanted to send my initial tissue sample to a company called Foundation One for comprehensive biomarker testing, in case future research identified a biomarker that I did have. When the test came back, we were pleasantly surprised that I had the ALK biomarker after all. I was THRILLED! I felt as though I had won the lung cancer lottery! Being diagnosed ALK+ meant I had the chance to take targeted therapy—giving me more options for my treatment plan.
Learning about my brain metastases
I started on crizotinib after my cancer spread following my first and second lines of treatment. After joining an online patient group, I learned that crizotinib is not effective in the brain, and that I should have a brain MRI at least every six months. I scheduled a brain MRI even though I didn’t have symptoms of the cancer spreading to my brain like dizziness, trouble speaking, or balance issues. During that scan, they discovered that I had seven new spots on my brain.
Finding a path forward with brain metastases
I met with three different radiation oncologists, who all wanted me to have whole brain radiation therapy (WBR). This was in February 2015 and alectinib and brigatinib were both still in clinical trials. After much thought, I joined the brigatinib trial in hopes it would diminish my brain mets and allow me to avoid whole brain radiation. I had twenty-eight glorious months on brigatinib before I had progression to my brain again. This time the brain mets (lung cancer that has spread to the brain) were too numerous to count. My oncologist recommended I travel to Boston to join Dr. Shaw's clinical trial of lorlatinib.
My first experience with brain radiation
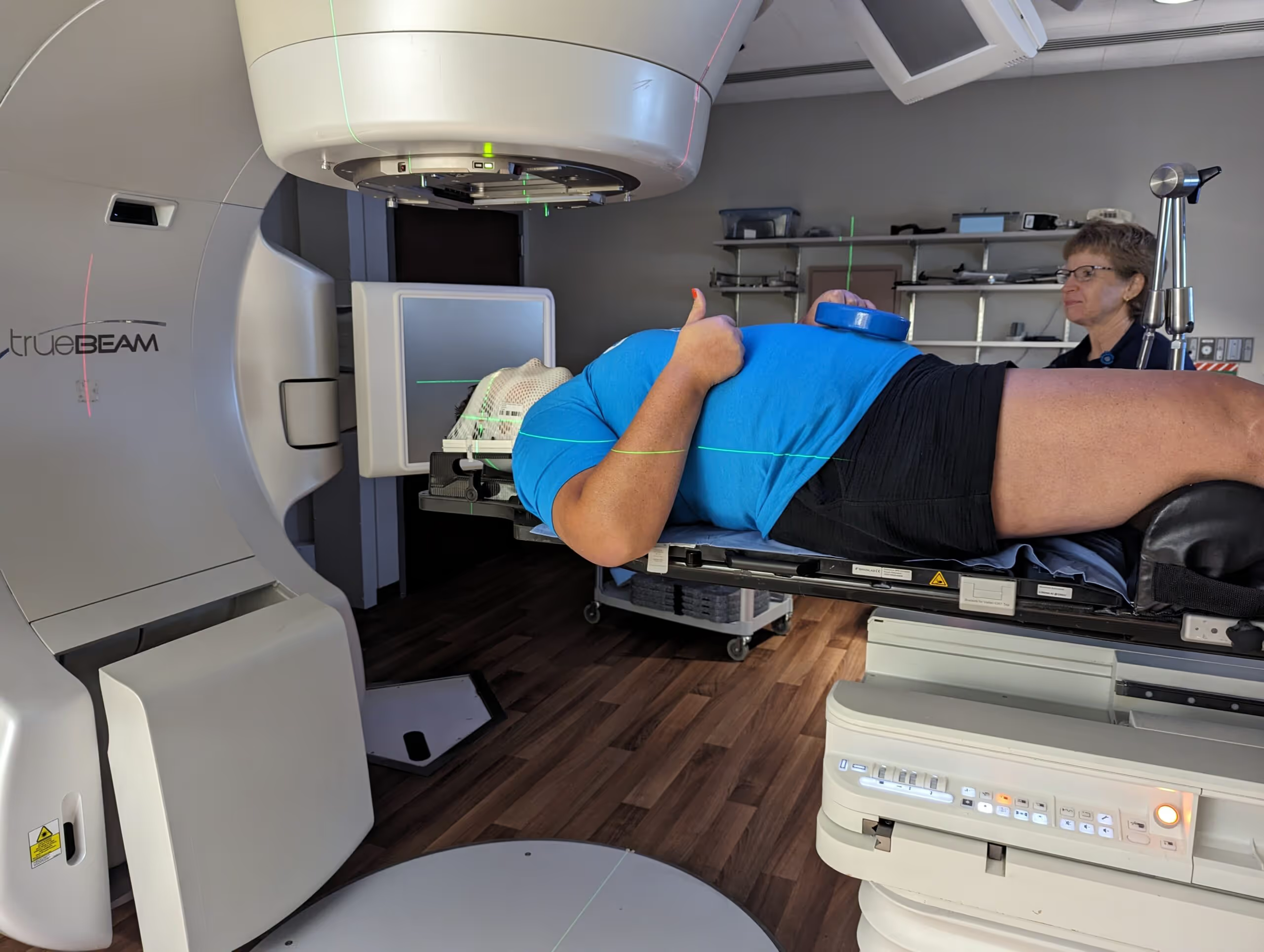
In July 2017, I started on a lorlatinib clinical trial, dodging brain radiation again. In May of 2018, I had mapping and a mold done for stereotactic radiosurgery (SRS). This is a very precisely aimed radiation beam that can treat the one spot on my brain instead of radiating the whole brain. The mold was made from my mouth, as that is how I was attached to the SRS machine. I had one spot in my brain that was not responding to lorlatinib and it was radiated. SRS was painless. I know it sounds strange, but I didn't mind being bolted to the machine because everything was very well explained to me by the nurses and doctors. The procedure went according to plan and I felt nothing.
Continued treatment with brain radiation

A year after SRS, the spot that was radiated showed growth. I had surgery in June 2019, followed by ten rounds of focused brain radiation on the growing spot. In preparation, I was fitted with a mask. The mask bolted into the radiation machine to keep me very still. Each session only lasted about 10 minutes a day. It took longer to change into the gown and get into the machine than it took to do the actual radiation. I was lucky and felt nothing more than a warming sensation and did not have any additional side effects. The treatment was successful, and I did not have any brain mets since the radiation until very recently.
Where I am today
I am lucky that my lung cancer mets continue to be stable in my spine and chest, but last month my care team discovered one on my left optic nerve (a very unusual place) so I needed to have focused brain radiation again. Thankfully I did not have any symptoms, but since it grew so fast, we had to act quickly. I completed five total treatments at the end of June and am continuing to take lorlatinib. Even though I'm retired from my music teaching career, I volunteer at my local school. I also lead worship music at my church. My lung cancer advocacy work has taken me all over the world and I wouldn’t change one thing. I only wish I was able to do more. All things considered, I believe I am blessed to be alive ten years after my diagnosis. I have been in two clinical trials and I'm on my sixth line of treatment with high hopes that research will catch up with me and there will be another therapy waiting for me as I need one.

May 30, 2023
By GO2 Senior Director, Support Initiatives, Maureen Rigney, LICSW [caption id="attachment_28132" align="alignright" width="340"]

Win Boerckel receiving GO2’s inaugural Lung Cancer Support Group Facilitator Award in 2009[/caption]Treasured GO2 friend and staunch lung cancer advocate, Winfield Boerckel, died in May following a diagnosis of brain cancer. Some of you may have had the pleasure of meeting or working with Win over the years. A social worker at CancerCare since 1996, Win ran a lung cancer support group on Long Island from 1997 until his retirement at the end of 2022. He was frequently called upon to share the perspectives of the lung cancer community on advisory boards and presented regularly at national and international conferences. Win’s first wife, Mary, died from cancer in 1982. He turned that difficult experience into further service by getting his master’s in social work, followed by his long career at CancerCare. His dedication to lung cancer was recognized in many ways, including receiving GO2’s inaugural Lung Cancer Support Group Facilitator Award in 2009, being nominated for CURE’s Lung Cancer Heroes Award in 2020 and being recognized for his 20-plus years of leadership to the Global Lung Cancer Coalition’s (GLCC) steering committee. You can read more about his expertise and commitment in the Lung Cancer Heroes 2020 essay book, starting on page 64. Everyone is more than their diagnosis or what they do for work. At his core, Win was a kind man with a great sense of humor. And he was impressive! He not only had an MSW but his MBA as well. He loved to bike. When we first met in 2007, he had just served as a team member on a Tour of Hope, a cross-country bike ride that raises awareness of the promise of cancer clinical trials and cancer research. [caption id="attachment_28134" align="alignright" width="248"]

Win with GLCC's achievement award[/caption]He was also an avid kayaker. Each year, he and his wife, Nancy, stayed at the same cabin in Maine for relaxation and kayaking. Win’s love of railroads made him a wonderful travel companion and I wish I remembered more of what he told me about all the different types of trains and tracks in our global travels with GLCC. The last time Win and I saw each other in person was in Vienna last September. Win introduced me to a beer spot he and Nancy loved, Stadboden. As usual, we talked about everything under the sun. By then, we were also both doing Wordle and talked strategy and shared with whom we relayed daily Wordle triumphs and defeats. Since 2021, most mornings I wondered if Win and I were doing the mini crossword at the same time. Now, every day, those games are a daily reminder of the friend I love. Thank you, Win, for your service to the lung cancer community.


November 22, 2022

When Heidi Hanson was diagnosed with stage 4 metastatic small cell lung cancer (SCLC) in December 2021, it wasn’t the typical story. Heidi had been suffering from headaches and dizziness which sent her to the emergency room. It was there that she was told surgery was needed to remove a tumor on her brain. When doctors tested the tumor they discovered that her cancer started in her lungs - she had small cell lung cancer and it spread to her brain.This wasn’t the first time that Heidi heard the words, “you have cancer.” Earlier in life, she was successfully treated for unrelated breast and bladder cancers. With her signature energy and positivity, she jokingly says that she’s had the “3 Bs: breast, bladder and brain cancers.”Heidi’s been treated for her small cell lung cancer with chemo, radiation and an immunotherapy drug called Tecentriq. Her first follow-up PET scan showed only one spot on her lung, which was treated with radiation. Her second follow-up PET scan showed no evidence of disease! She’s currently continuing Tecentriq with close monitoring.We talked to Hanson about inspiration, where she finds strength and her advice for people who are newly diagnosed with lung cancer.Maintain a positive attitude, keep moving, and ask for help.Hanson believes you must be honest about how you’re feeling. “It’s okay to say you’re scared. It’s okay to say you don’t know how you feel. It’s okay to wallow around and feel depressed—but don’t stay there.” She notes that while it’s helpful to be positive, you have to give yourself permission to feel down every now and then.Hanson added that she also follows her doctor’s orders —eats small meals of healthy foods, drinks a lot of water, limits sweets and gets plenty of exercise. Hanson said, “No matter how I feel, I walk. Moving and exercise help to keep my body and mind healthy.”Most importantly, Hanson emphasized that you can’t fight lung cancer alone. “When people want to do something for you, let them,” she stressed. “And don’t be afraid to ask for help. Talk to a therapist or a good friend when you need support.”Do your research—and be your own advocate.“I’m not afraid of lung cancer,” said Hanson, “and I stand up for what I do and don’t want.”She explained that she did her research and chose a doctor she trusts. Her advice to others diagnosed with SCLC is to read and learn all you can so that you can walk into your doctor’s office with confidence—and your questions. “Find out where to get the best treatment, who is the best person to see, and how to get a second opinion,” she said. “You find peace of mind when you have the right care.”Live in the present.Hanson advises other people diagnosed with lung cancer to live in the present moment. “I’ve found it is best not to look too far into the future,” she said. “Just get up and go today. Take it one day at a time and don’t put off the things that are important to you.”We are excited to bring you more stories about living with lung cancer in upcoming issues of Your Community, including features about survivorship, wellness, and practical tips about living well with lung cancer. If you have ideas on topics or stories you’d like to read about here, please email yourcommunity@go2.org.
