What is immunotherapy for lung cancer?
Immunotherapy is a type of cancer treatment that helps your body’s own immune system find and attack cancer cells. This type of cancer treatment works by boosting the immune system directly or preventing how cancer cells hide from the immune system.
Your healthcare team will determine whether immunotherapy is right for you based on your stage of cancer, other treatments you’re receiving, overall health, and biomarker testing results, if applicable.
Immunotherapy is available for both people living with non-small cell lung cancer (NSCLC) and small cell lung cancer (SCLC).
How does immunotherapy for non-small cell lung cancer (NSCLC) work?
To understand how immunotherapy for NSCLC works, you need to know a little bit about the immune system. Your immune system protects your body against germs and diseases that can make you sick. Most of the time, it knows which cells in the body are normal and healthy and which cells are not healthy. This allows it to attack disease and germ cells without attacking healthy cells.
When your immune system finds cancer cells, it goes to work to destroy them. Sometimes it has trouble finding cancer cells because they can hide and appear like healthy cells. Cancer cells hide from the immune system by attaching themselves to immune cells. Staying attached to immune cells slows down or stops the ability of the immune cells to attack the cancer cells.
The place on the cells where the cancer and immune cells attach to each other is called a checkpoint. There are proteins on the surface of each cell that attach the immune cell and the cancer cell together.
- The protein on the immune cell is called PD-1 or CTLA-4.
- The protein on the cancer cell is called PD-L1.
By staying attached to the immune cells, it slows down or stops the ability of the immune cell to attack the cancer cell. Immunotherapy works to block cancer cells from attaching to immune cells, leaving the cancer cells exposed and allowing the immune system to attack them.
Checkpoint inhibitors
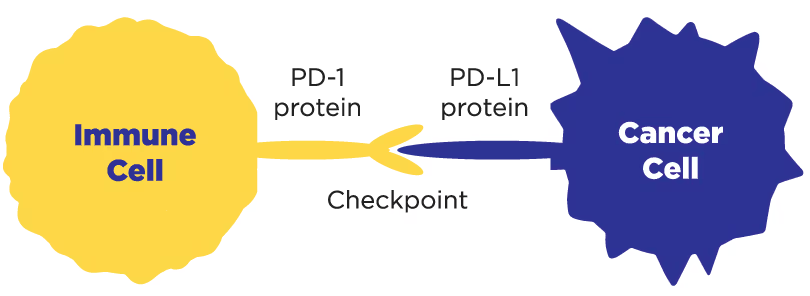
Checkpoint inhibitors are a type of immunotherapy that works by blocking cancer cells from attaching to immune cells. This prevents them from hiding from the immune system, and allows the immune system to attack cancer cell more effectively.
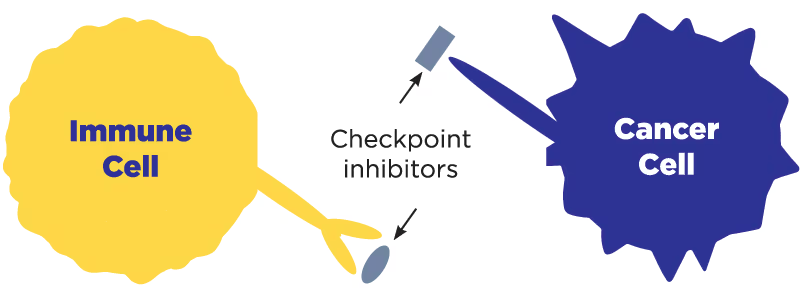
Immunotherapy drugs for NSCLC
All people diagnosed with NSCLC stages 1B through 4B (stages IB through IVB) should ask for comprehensive biomarker testing to receive the best treatment for their specific type of cancer. This is because some cancer drugs work by finding specific targets or protiens in cancer cells, called biomarkers. Comprehensive biomarker testing looks for a wide variety of biomarkers to find the cancer treatment that is best for that specific cancer type and subtype.
A useful biomarker for immunotherapy in NSCLC is the amount of the protein PD-L1 that cancer cells have on their surface. The amount of PD-L1 can help predict how well the cancer may respond to a PD-1 or PD-L1 checkpoint inhibitor. Research is ongoing to learn more about these biomarkers and their relationship to immunotherapy treatment. Ask your healthcare team if you’ve had biomarker testing and how the results are being used in your treatment plan.
Common NSCLC immunotherapy checkpoint inhibitor drugs include:
Imfinzi (durvalumab)
Blocking the PD-L1 protein on the cancer cell
Jemperli (dostarlimab)
Blocking the PD-L1 protein on the cancer cell
Keytruda (pembrolizumab)
Blocking the PD-L1 protein on the immune cell
Libtayo (cemiplimab-rwlc)
Blocking the PD-L1 protein on the immune cell
Opdivo (nivolumab)
Blocking the PD-1 protein on the immune cell
Tecentriq (atezolizumab)
Blocking the PD-L1 protein on the immune cell
Imjudo (tremelimumab)
Blocking the CTLA-4 protein on the immune cell
Yervoy (ipilimumab)
Blocking the CTLA-4 protein on the immune cell
Immunotherapy side effects for NSCLC
Since immunotherapy activates your immune system, healthy cells in your body can also be affected when there is an overresponse from the immune system. Some side effects are caused by this over-response.
The side effects you may experience depend on the type of immunotherapy you receive, how long you receive it, and your body’s individual response. It is always important to talk to your healthcare team about ways to manage side effects before you have them. They can often be prevented, treated, or eased with medicines or palliative care.
Lung cancer immunotherapy drugs can cause short and long-term side effects and some can be severe.
Common side effects may include:
- Aching joints and muscles
- Constipation and/or diarrhea
- Coughing
- Trouble sleeping and/or feeling tired
- Loss of appetite
- Mouth sores
- Skin reactions
- Throat soreness
Since immunotherapy increases the activity in the immune system, healthy cells are sometimes attacked causing inflammation in healthy tissue. Some more serious side effects are caused by organ inflammation.
Contact your healthcare team right away if you have any of these symptoms:
- Chest pain, trouble breathing, dizziness, confusion, or fainting
- Diarrhea with cramps or pain, blood in the stool or urine, or dark urine
- A fever of 100.5 degrees Farenehit or above
- Changes in vision, memory, or thinking skills
- Swelling in any part of the body
How does immunotherapy for small cell lung cancer (SCLC) work?
To understand how immunotherapy for SCLC works, you need to know a little bit about the immune system. Your immune system protects your body against germs and diseases that can make you sick. Most of the time, it knows which cells in the body are normal and healthy and which cells are not healthy. This allows it to attack disease and germ cells without attacking healthy cells.
When your immune system finds cancer cells, it goes to work to destroy them. Sometimes it has trouble finding cancer cells because they can appear like healthy cells. Immunotherapy works to help your immune system find and attack cancer cells.
There are 2 types of immunotherapies approved for SCLC: checkpoint inhibitors and T-cell engagers. They each work in very different ways and are used at different points in treatment.
Checkpoint inhibitors
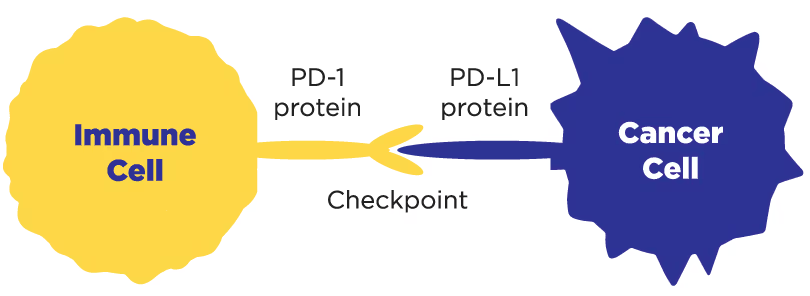
Cancer cells can hide from the immune system by attaching themselves to immune cells. Staying attached to immune cells slows down or stops the ability of the immune cells to attack the cancer cells.
The place on the cells where the cancer and immune cellsattach to each other is called a checkpoint. There are proteins on the surface of each cell that attach the immune cell and the cancer cell together.
- The protein on the immune cell is called PD-1.
- The protein on the cancer cell is caled PD-L1.
By staying attached to the immune cells, it slows down or stops the ability of the immune cell to attack the cancer cell. Immunotherapy works to block cancer cells from attaching to immune cells, leaving the cancer cells exposed and allowing the immune system to attack them.
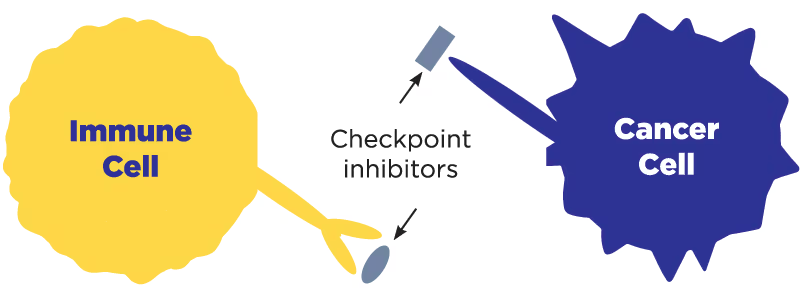
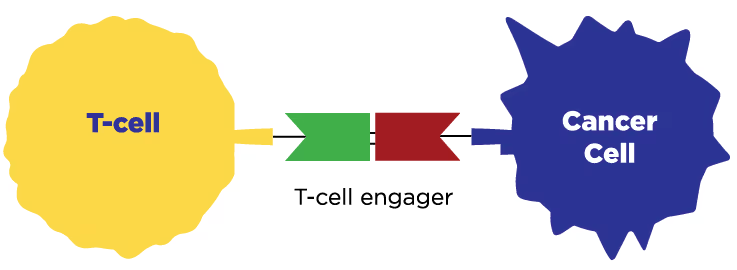
T-cell engagers
A T-cell is a type of immune cells that helps to protect the body from diseases like cancer. T-cell engagers work by connecting a T-cell to a cancer cell, which causes the T-cell to activate and kill the cancer cell. This connection helps your immune system to find and attack the cancer.
Immunotherapy drugs for SCLC
Your healthcare team will determine whether immunotherapy is right for you based on your stage of cancer, the timing of other treatments you may need, and your overall health.
Common SCLC immunotherapy drugs include:
Imfinzi (durvalumab)
Blocking the PD-L1 protein on the cancer cell
Tecentriq (atezolizumab)
Blocking the PD-L1 protein on the cancer cell
Imdelltra (tarlatamab-dlle)
Connecting T-cells with cancer cells
Immunotherapy side effects for SCLC
Since immunotherapy activates your immune system, healthy cells in your body can also be affected when there is an over-response from the immune system. Some side effects are caused by this over-response.
The side effects of immunotherapy you may experience depend on the type of immunotherapy you receive, how long you receive it, and your body’s individual response. It is always important to talk to your healthcare team about ways to manage side effects before you have them. They can often be prevented, treated, or eased with medicines or palliative care.
Short- and long-term side effects can happen due to immunotherapy drugs for lung cancer. Knowing what to expect can help you prepare for a better treatment experience.
Common side effects may include:
- Aching joints and muscles
- Constipation and/or diarrhea
- Coughing
- Trouble sleeping and/or feeling tired
- Loss of appetite
- Mouth sores
- Skin reactions
- Throat soreness
Since immunotherapy increases the activity in the immune system, healthy cells are sometimes attacked causing inflammation in healthy tissue. Some more serious side effects are caused by organ inflammation.
Contact your healthcare team right away if you have any of these symptoms:
- Chest pain, trouble breathing, dizziness, confusion, or fainting
- Diarrhea with cramps or pain, blood in the stool or urine, or dark urine
- A fever of 100.5 degrees Farhenheit or above
- Changes in vision, memory, or thinking skills
- Swelling in any part of the body
What should I know about T-cell engager side effects?
T-cell engagers can cause more serious side effects such as cytokine release syndrome (CRS) and/or immune effector cell-associated neurotoxicity syndrome (ICANS). It’s very important to ask your healthcare team for the full list of signs of these conditions and contact them right away if they occur.
CRS is a common side effect of immunotherapy treatment that can be serious or life-threatening. It can occur when the immune system releases a high number of an immune substance called cytokines as an over-response to T-cell engagers. When this happens, too much inflammation occurs, which can affect how your body’s organs are able to work.
CRS can cause a range of symptoms from mild to severe including fever, headache, nausea, and trouble breathing, If CRS is not treated right away, it can progress to very low blood pressure and other life-threatening issues.
Another potentially life-threatening complication of T-cell engager immunotherapy is ICANS. It can happen with or without CRS and can happen before, during, or after CRS. It can occur days or weeks after receiving T-cell engager treatment.
ICANS affects how your brain works and impacts your ability to think, speak, and move. Symptoms can include weakness, confusion, difficulty talking, or problems with balance.
Contact your healthcare team right away if you experience any of these symptoms.
Questions to ask your healthcare team about lung cancer immunotherapy
Talking with your healthcare team and asking questions ensures you stay informed about your condition and are an active participant in your treatment. The following sample questions can help get the conversation going:
- What immunotherapy treatment do you recommend for me and why?
- What possible side effects might I have, and how can I handle them?
- When do I start treatment? How long will it last?
- Are there any clinical trials that are right for me? If so, how do I learn more about them?
Explore other questions to ask your healthcare team.
Recent advancements in lung cancer
Explore recent advancements in lung cancer, new treatment approvals, research breakthroughs, and more by signing up for GO2’s email communications.

Frequently asked questions
Where can I find more resources and support?
Contact the GO2 HelpLine at 1-800-298-2436 or email support@go2.org to connect with caring and highly trained staff who listen, answer your questions, and provide support. We offer many free programs and educational resources to meet your needs.
How is immunotherapy given?
Some immunotherapy drugs are given through a IV or a port (a tube placed in a vein) while others can be injected with a needle just under the skin. Treatments usually take a few minutes, with a few weeks between each one. However, there are a few immunotherapy drugs that are approved for use as an injection. This means the drug can be injected through the skin, which requires less treatment time.
Why do lung cancer tumors look bigger after starting immunotherapy?
It is common for a tumor to get bigger during the early stage of immunotherapy treatment. This happens when the medication causes the immune system to attack the cancer cells, filling them with immune cells.
Will immunotherapy for lung cancer prevent me from getting other sicknesses?
No. While lung cancer immunotherapy is designed to help attack the cancer by activating your immune system, it does not provide the protection to prevent or fight other illnesses.
Where can I find support and resources for lung cancer treatment?
Contact the GO2 HelpLine at 1-800-298-2436 or email support@go2.org to connect with caring and highly trained staff who listen, answer your questions, and provide support. In addition to our HelpLine, we have free educational materials that can be downloaded or ordered from our online store. You can also join our Phone Buddy program to connect with someone who is living with lung cancer or Gathering HOPE, for group support.
